An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- v.369; 2020

Food for Thought 2020
Food and mood: how do diet and nutrition affect mental wellbeing, joseph firth.
1 Division of Psychology and Mental Health, Faculty of Biology, Medicine and Health, Oxford Road, University of Manchester, Manchester M13 9PL, UK
2 NICM Health Research Institute, Western Sydney University, Westmead, Australia
James E Gangwisch
3 Department of Psychiatry, Columbia University Vagelos College of Physicians and Surgeons, New York, USA
4 New York State Psychiatric Institute, New York, NY, USA
Alessandra Borsini
5 Section of Stress, Psychiatry and Immunology Laboratory, Institute of Psychiatry, Psychology and Neuroscience, Department of Psychological Medicine, King’s College London, London, UK
Robyn E Wootton
6 School of Psychological Science, University of Bristol, Bristol, UK
7 MRC Integrative Epidemiology Unit, Oakfield House, Bristol, UK
8 NIHR Biomedical Research Centre, University Hospitals Bristol NHS Foundation Trust and University of Bristol, Bristol, UK
Emeran A Mayer
9 G Oppenheimer Center for Neurobiology of Stress and Resilience, UCLA Vatche and Tamar Manoukian Division of Digestive Diseases, UCLA, Los Angeles, CA, USA
10 UCLA Microbiome Center, David Geffen School of Medicine, UCLA, Los Angeles, CA, USA
Poor nutrition may be a causal factor in the experience of low mood, and improving diet may help to protect not only the physical health but also the mental health of the population, say Joseph Firth and colleagues
Key messages
- Healthy eating patterns, such as the Mediterranean diet, are associated with better mental health than “unhealthy” eating patterns, such as the Western diet
- The effects of certain foods or dietary patterns on glycaemia, immune activation, and the gut microbiome may play a role in the relationships between food and mood
- More research is needed to understand the mechanisms that link food and mental wellbeing and determine how and when nutrition can be used to improve mental health
Depression and anxiety are the most common mental health conditions worldwide, making them a leading cause of disability. 1 Even beyond diagnosed conditions, subclinical symptoms of depression and anxiety affect the wellbeing and functioning of a large proportion of the population. 2 Therefore, new approaches to managing both clinically diagnosed and subclinical depression and anxiety are needed.
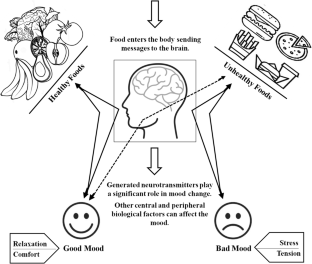
In recent years, the relationships between nutrition and mental health have gained considerable interest. Indeed, epidemiological research has observed that adherence to healthy or Mediterranean dietary patterns—high consumption of fruits, vegetables, nuts, and legumes; moderate consumption of poultry, eggs, and dairy products; and only occasional consumption of red meat—is associated with a reduced risk of depression. 3 However, the nature of these relations is complicated by the clear potential for reverse causality between diet and mental health ( fig 1 ). For example, alterations in food choices or preferences in response to our temporary psychological state—such as “comfort foods” in times of low mood, or changes in appetite from stress—are common human experiences. In addition, relationships between nutrition and longstanding mental illness are compounded by barriers to maintaining a healthy diet. These barriers disproportionality affect people with mental illness and include the financial and environmental determinants of health, and even the appetite inducing effects of psychiatric medications. 4

Hypothesised relationship between diet, physical health, and mental health. The dashed line is the focus of this article.
While acknowledging the complex, multidirectional nature of the relationships between diet and mental health ( fig 1 ), in this article we focus on the ways in which certain foods and dietary patterns could affect mental health.
Mood and carbohydrates
Consumption of highly refined carbohydrates can increase the risk of obesity and diabetes. 5 Glycaemic index is a relative ranking of carbohydrate in foods according to the speed at which they are digested, absorbed, metabolised, and ultimately affect blood glucose and insulin levels. As well as the physical health risks, diets with a high glycaemic index and load (eg, diets containing high amounts of refined carbohydrates and sugars) may also have a detrimental effect on psychological wellbeing; data from longitudinal research show an association between progressively higher dietary glycaemic index and the incidence of depressive symptoms. 6 Clinical studies have also shown potential causal effects of refined carbohydrates on mood; experimental exposure to diets with a high glycaemic load in controlled settings increases depressive symptoms in healthy volunteers, with a moderately large effect. 7
Although mood itself can affect our food choices, plausible mechanisms exist by which high consumption of processed carbohydrates could increase the risk of depression and anxiety—for example, through repeated and rapid increases and decreases in blood glucose. Measures of glycaemic index and glycaemic load can be used to estimate glycaemia and insulin demand in healthy individuals after eating. 8 Thus, high dietary glycaemic load, and the resultant compensatory responses, could lower plasma glucose to concentrations that trigger the secretion of autonomic counter-regulatory hormones such as cortisol, adrenaline, growth hormone, and glucagon. 5 9 The potential effects of this response on mood have been examined in experimental human research of stepped reductions in plasma glucose concentrations conducted under laboratory conditions through glucose perfusion. These findings showed that such counter-regulatory hormones may cause changes in anxiety, irritability, and hunger. 10 In addition, observational research has found that recurrent hypoglycaemia (low blood sugar) is associated with mood disorders. 9
The hypothesis that repeated and rapid increases and decreases in blood glucose explain how consumption of refined carbohydrate could affect psychological state appears to be a good fit given the relatively fast effect of diets with a high glycaemic index or load on depressive symptoms observed in human studies. 7 However, other processes may explain the observed relationships. For instance, diets with a high glycaemic index are a risk factor for diabetes, 5 which is often a comorbid condition with depression. 4 11 While the main models of disease pathophysiology in diabetes and mental illness are separate, common abnormalities in insulin resistance, brain volume, and neurocognitive performance in both conditions support the hypothesis that these conditions have overlapping pathophysiology. 12 Furthermore, the inflammatory response to foods with a high glycaemic index 13 raises the possibility that diets with a high glycaemic index are associated with symptoms of depression through the broader connections between mental health and immune activation.
Diet, immune activation, and depression
Studies have found that sustained adherence to Mediterranean dietary patterns can reduce markers of inflammation in humans. 14 On the other hand, high calorie meals rich in saturated fat appear to stimulate immune activation. 13 15 Indeed, the inflammatory effects of a diet high in calories and saturated fat have been proposed as one mechanism through which the Western diet may have detrimental effects on brain health, including cognitive decline, hippocampal dysfunction, and damage to the blood-brain barrier. 15 Since various mental health conditions, including mood disorders, have been linked to heightened inflammation, 16 this mechanism also presents a pathway through which poor diet could increase the risk of depression. This hypothesis is supported by observational studies which have shown that people with depression score significantly higher on measures of “dietary inflammation,” 3 17 characterised by a greater consumption of foods that are associated with inflammation (eg, trans fats and refined carbohydrates) and lower intakes of nutritional foods, which are thought to have anti-inflammatory properties (eg, omega-3 fats). However, the causal roles of dietary inflammation in mental health have not yet been established.
Nonetheless, randomised controlled trials of anti-inflammatory agents (eg, cytokine inhibitors and non-steroidal anti-inflammatory drugs) have found that these agents can significantly reduce depressive symptoms. 18 Specific nutritional components (eg, polyphenols and polyunsaturated fats) and general dietary patterns (eg, consumption of a Mediterranean diet) may also have anti-inflammatory effects, 14 19 20 which raises the possibility that certain foods could relieve or prevent depressive symptoms associated with heightened inflammatory status. 21 A recent study provides preliminary support for this possibility. 20 The study shows that medications that stimulate inflammation typically induce depressive states in people treated, and that giving omega-3 fatty acids, which have anti-inflammatory properties, before the medication seems to prevent the onset of cytokine induced depression. 20
However, the complexity of the hypothesised three way relation between diet, inflammation, and depression is compounded by several important modifiers. For example, recent clinical research has observed that stressors experienced the previous day, or a personal history of major depressive disorders, may cancel out the beneficial effects of healthy food choices on inflammation and mood. 22 Furthermore, as heightened inflammation occurs in only some clinically depressed individuals, anti-inflammatory interventions may only benefit certain people characterised by an “inflammatory phenotype,” or those with comorbid inflammatory conditions. 18 Further interventional research is needed to establish if improvements in immune regulation, induced by diet, can reduce depressive symptoms in those affected by inflammatory conditions.
Brain, gut microbiome, and mood
A more recent explanation for the way in which our food may affect our mental wellbeing is the effect of dietary patterns on the gut microbiome—a broad term that refers to the trillions of microbial organisms, including bacteria, viruses, and archaea, living in the human gut. The gut microbiome interacts with the brain in bidirectional ways using neural, inflammatory, and hormonal signalling pathways. 23 The role of altered interactions between the brain and gut microbiome on mental health has been proposed on the basis of the following evidence: emotion-like behaviour in rodents changes with changes in the gut microbiome, 24 major depressive disorder in humans is associated with alterations of the gut microbiome, 25 and transfer of faecal gut microbiota from humans with depression into rodents appears to induce animal behaviours that are hypothesised to indicate depression-like states. 25 26 Such findings suggest a role of altered neuroactive microbial metabolites in depressive symptoms.
In addition to genetic factors and exposure to antibiotics, diet is a potentially modifiable determinant of the diversity, relative abundance, and functionality of the gut microbiome throughout life. For instance, the neurocognitive effects of the Western diet, and the possible mediating role of low grade systemic immune activation (as discussed above) may result from a compromised mucus layer with or without increased epithelial permeability. Such a decrease in the function of the gut barrier is sometimes referred to as a “leaky gut” and has been linked to an “unhealthy” gut microbiome resulting from a diet low in fibre and high in saturated fats, refined sugars, and artificial sweeteners. 15 23 27 Conversely, the consumption of a diet high in fibres, polyphenols, and unsaturated fatty acids (as found in a Mediterranean diet) can promote gut microbial taxa which can metabolise these food sources into anti-inflammatory metabolites, 15 28 such as short chain fatty acids, while lowering the production of secondary bile acids and p-cresol. Moreover, a recent study found that the ingestion of probiotics by healthy individuals, which theoretically target the gut microbiome, can alter the brain’s response to a task that requires emotional attention 29 and may even reduce symptoms of depression. 30 When viewed together, these studies provide promising evidence supporting a role of the gut microbiome in modulating processes that regulate emotion in the human brain. However, no causal relationship between specific microbes, or their metabolites, and complex human emotions has been established so far. Furthermore, whether changes to the gut microbiome induced by diet can affect depressive symptoms or clinical depressive disorders, and the time in which this could feasibly occur, remains to be shown.
Priorities and next steps
In moving forward within this active field of research, it is firstly important not to lose sight of the wood for the trees—that is, become too focused on the details and not pay attention to the bigger questions. Whereas discovering the anti-inflammatory properties of a single nutrient or uncovering the subtleties of interactions between the gut and the brain may shed new light on how food may influence mood, it is important not to neglect the existing knowledge on other ways diet may affect mental health. For example, the later consequences of a poor diet include obesity and diabetes, which have already been shown to be associated with poorer mental health. 11 31 32 33 A full discussion of the effect of these comorbidities is beyond the scope of our article (see fig 1 ), but it is important to acknowledge that developing public health initiatives that effectively tackle the established risk factors of physical and mental comorbidities is a priority for improving population health.
Further work is needed to improve our understanding of the complex pathways through which diet and nutrition can influence the brain. Such knowledge could lead to investigations of targeted, even personalised, interventions to improve mood, anxiety, or other symptoms through nutritional approaches. However, these possibilities are speculative at the moment, and more interventional research is needed to establish if, how, and when dietary interventions can be used to prevent mental illness or reduce symptoms in those living with such conditions. Of note, a recent large clinical trial found no significant benefits of a behavioural intervention promoting a Mediterranean diet for adults with subclinical depressive symptoms. 34 On the other hand, several recent smaller trials in individuals with current depression observed moderately large improvements from interventions based on the Mediterranean diet. 35 36 37 Such results, however, must be considered within the context of the effect of people’s expectations, particularly given that individuals’ beliefs about the quality of their food or diet may also have a marked effect on their sense of overall health and wellbeing. 38 Nonetheless, even aside from psychological effects, consideration of dietary factors within mental healthcare may help improve physical health outcomes, given the higher rates of cardiometabolic diseases observed in people with mental illness. 33
At the same time, it is important to be remember that the causes of mental illness are many and varied, and they will often present and persist independently of nutrition and diet. Thus, the increased understanding of potential connections between food and mental wellbeing should never be used to support automatic assumptions, or stigmatisation, about an individual’s dietary choices and their mental health. Indeed, such stigmatisation could be itself be a casual pathway to increasing the risk of poorer mental health. Nonetheless, a promising message for public health and clinical settings is emerging from the ongoing research. This message supports the idea that creating environments and developing measures that promote healthy, nutritious diets, while decreasing the consumption of highly processed and refined “junk” foods may provide benefits even beyond the well known effects on physical health, including improved psychological wellbeing.
Contributors and sources: JF has expertise in the interaction between physical and mental health, particularly the role of lifestyle and behavioural health factors in mental health promotion. JEG’s area of expertise is the study of the relationship between sleep duration, nutrition, psychiatric disorders, and cardiometabolic diseases. AB leads research investigating the molecular mechanisms underlying the effect of stress and inflammation on human hippocampal neurogenesis, and how nutritional components and their metabolites can prevent changes induced by those conditions. REW has expertise in genetic epidemiology approaches to examining casual relations between health behaviours and mental illness. EAM has expertise in brain and gut interactions and microbiome interactions. All authors contributed to, read, and approved the paper, and all the information was sourced from articles published in peer reviewed research journals. JF is the guarantor.
Competing interests: We have read and understood BMJ policy on declaration of interests and declare the following: JF is supported by a University of Manchester Presidential Fellowship and a UK Research and Innovation Future Leaders Fellowship and has received support from a NICM-Blackmores Institute Fellowship. JEG served on the medical advisory board on insomnia in the cardiovascular patient population for the drug company Eisai. AB has received research funding from Johnson & Johnson for research on depression and inflammation, the UK Medical Research Council, the European Commission Horizon 2020, the National Institute for Health Research (NIHR) Biomedical Research Centre at South London and Maudsley NHS Foundation Trust, and King’s College London. REW receives funding from the National Institute for Health Research Biomedical Research Centre at the University Hospitals Bristol NHS Foundation Trust and the University of Bristol. EAM has served on the external advisory boards of Danone, Viome, Amare, Axial Biotherapeutics, Pendulum, Ubiome, Bloom Science, Mahana Therapeutics, and APC Microbiome Ireland, and he receives royalties from Harper & Collins for his book The Mind Gut Connection. He is supported by grants from the National Institute of Diabetes and Digestive and Kidney Diseases, and the US Department of Defense. The views expressed are those of the authors and not necessarily those of the organisations above.
Provenance and peer review: Commissioned; externally peer reviewed.
This article is part of series commissioned by The BMJ. Open access fees are paid by Swiss Re, which had no input into the commissioning or peer review of the articles. T he BMJ thanks the series advisers, Nita Forouhi, Dariush Mozaffarian, and Anna Lartey for valuable advice and guiding selection of topics in the series.
Food and mood: how do diet and nutrition affect mental wellbeing?
Affiliations.
- 1 Division of Psychology and Mental Health, Faculty of Biology, Medicine and Health, Oxford Road, University of Manchester, Manchester M13 9PL, UK [email protected].
- 2 NICM Health Research Institute, Western Sydney University, Westmead, Australia.
- 3 Department of Psychiatry, Columbia University Vagelos College of Physicians and Surgeons, New York, USA.
- 4 New York State Psychiatric Institute, New York, NY, USA.
- 5 Section of Stress, Psychiatry and Immunology Laboratory, Institute of Psychiatry, Psychology and Neuroscience, Department of Psychological Medicine, King's College London, London, UK.
- 6 School of Psychological Science, University of Bristol, Bristol, UK.
- 7 MRC Integrative Epidemiology Unit, Oakfield House, Bristol, UK.
- 8 NIHR Biomedical Research Centre, University Hospitals Bristol NHS Foundation Trust and University of Bristol, Bristol, UK.
- 9 G Oppenheimer Center for Neurobiology of Stress and Resilience, UCLA Vatche and Tamar Manoukian Division of Digestive Diseases, UCLA, Los Angeles, CA, USA.
- 10 UCLA Microbiome Center, David Geffen School of Medicine, UCLA, Los Angeles, CA, USA.
- PMID: 32601102
- PMCID: PMC7322666
- DOI: 10.1136/bmj.m2382
Poor nutrition may be a causal factor in the experience of low mood, and improving diet may help to protect not only the physical health but also the mental health of the population, say Joseph Firth and colleagues
- Anxiety / diet therapy*
- Anxiety / immunology
- Anxiety / prevention & control
- Cognition / physiology*
- Depression / diet therapy*
- Depression / immunology
- Depression / prevention & control
- Diet, Healthy*
- Gastrointestinal Microbiome / immunology*
- Inflammation / diet therapy*
- Inflammation / immunology
- Inflammation / prevention & control
- Nutritional Physiological Phenomena
- Nutritional Status
Grants and funding
- MR/T021780/1/MRC_/Medical Research Council/United Kingdom
- Share full article
Advertisement
Supported by
How Food May Improve Your Mood
The sugar-laden, high-fat foods we often crave when we are stressed or depressed, as comforting as they are, may be the least likely to benefit our mental health.

By Anahad O’Connor
As people across the globe grappled with higher levels of stress, depression and anxiety this past year , many turned to their favorite comfort foods: ice cream, pastries, pizza, hamburgers. But studies in recent years suggest that the sugar-laden and high-fat foods we often crave when we are stressed or depressed, as comforting as they may seem, are the least likely to benefit our mental health. Instead, whole foods such as vegetables, fruit, fish, eggs, nuts and seeds, beans and legumes and fermented foods like yogurt may be a better bet.
The findings stem from an emerging field of research known as nutritional psychiatry , which looks at the relationship between diet and mental wellness. The idea that eating certain foods could promote brain health, much the way it can promote heart health, might seem like common sense. But historically, nutrition research has focused largely on how the foods we eat affect our physical health, rather than our mental health. For a long time, the potential influence of food on happiness and mental well-being, as one team of researchers recently put it , was “virtually ignored.”
But over the years, a growing body of research has provided intriguing hints about the ways in which foods may affect our moods. A healthy diet promotes a healthy gut, which communicates with the brain through what is known as the gut-brain axis. Microbes in the gut produce neurotransmitters like serotonin and dopamine, which regulate our mood and emotions, and the gut microbiome has been implicated in mental health outcomes. “A growing body of literature shows that the gut microbiome plays a shaping role in a variety of psychiatric disorders, including major depressive disorder,” a team of scientists wrote in the Harvard Review of Psychiatry last year.
Large population studies, too, have found that people who eat a lot of nutrient-dense foods report less depression and greater levels of happiness and mental well-being . One such study, from 2016, that followed 12,400 people for about seven years found that those who increased their consumption of fruits and vegetables during the study period rated themselves substantially higher on questionnaires about their general levels of happiness and life satisfaction.
Large observational studies, however, can show only correlations, not causation, which raises the question: Which comes first? Do anxiety and depression drive people to choose unhealthy foods, or vice versa? Are people who are happy and optimistic more motivated to consume nutritious foods? Or does a healthy diet directly brighten their moods?
The first major trial to shed light on the food-mood connection was published in 2017 . A team of researchers wanted to know whether dietary changes would help alleviate depression , so they recruited 67 people who were clinically depressed and split them into groups. One group went to meetings with a dietitian who taught them to follow a traditional Mediterranean-style diet. The other group, serving as the control, met regularly with a research assistant who provided social support but no dietary advice.
At the start of the study, both groups consumed a lot of sugary foods , processed meats and salty snacks, and very little fiber, lean proteins or fruits and vegetables. But the diet group made big changes. They replaced candy, fast food and pastries with whole foods such as nuts, beans, fruits and legumes. They switched from white bread to whole grain and sourdough bread. They gave up sugary cereals and ate muesli and oatmeal. Instead of pizza, they ate vegetable stir-fries. And they replaced highly processed meats like ham, sausages and bacon with seafood and small amounts of lean red meats.
Importantly, both groups were counseled to continue taking any antidepressants or other medications they were prescribed. The goal of the study was not to see if a healthier diet could replace medication, but whether it could provide additional benefits like exercise, good sleep and other lifestyle behaviors.
After 12 weeks, average depression scores improved in both groups, which might be expected for anyone entering a clinical trial that provided additional support, regardless of which group you were in. But depression scores improved to a far greater extent in the group that followed the healthy diet: roughly a third of those people were no longer classified as depressed, compared to 8 percent of people in the control group.
The results were striking for a number of reasons. The diet benefited mental health even though the participants did not lose any weight. People also saved money by eating the more nutritious foods, demonstrating that a healthy diet can be economical. Before the study, the participants spent on average $138 per week on food. Those who switched to the healthy diet lowered their food costs to $112 per week.
The recommended foods were relatively inexpensive and available at most grocery stores. They included things like canned beans and lentils, canned salmon, tuna and sardines, and frozen and conventional produce, said Felice Jacka, the lead author of the study.
“Mental health is complex,” said Dr. Jacka, the director of the Food & Mood Centre at Deakin University in Australia and the president of the International Society for Nutritional Psychiatry Research. “Eating a salad is not going to cure depression. But there’s a lot you can do to lift your mood and improve your mental health, and it can be as simple as increasing your intake of plants and healthy foods.”
A number of randomized trials have reported similar findings . In one study of 150 adults with depression that was published last year, researchers found that people assigned to follow a Mediterranean diet supplemented with fish oil for three months had greater reductions in symptoms of depression, stress and anxiety after three months compared to a control group.
Still, not every study has had positive results. A large, yearlong trial published in JAMA in 2019, for example, found that a Mediterranean diet reduced anxiety but did not prevent depression in a group of people at high risk. Taking supplements such as vitamin D, selenium and omega-3 fatty acids had no impact on either depression or anxiety.
Most psychiatric professional groups have not adopted dietary recommendations, in part because experts say that more research is needed before they can prescribe a specific diet for mental health. But public health experts in countries around the world have started encouraging people to adopt lifestyle behaviors like exercise , sound sleep , a heart-healthy diet and avoiding smoking that may reduce inflammation and have benefits for the brain. The Royal Australian and New Zealand College of Psychiatrists issued clinical practice guidelines encouraging clinicians to address diet, exercise and smoking before starting patients on medication or psychotherapy.
Individual clinicians, too, are already incorporating nutrition into their work with patients. Dr. Drew Ramsey, a psychiatrist and assistant clinical professor at the Columbia University College of Physicians and Surgeons in New York, begins his sessions with new patients by taking their psychiatric history and then exploring their diet. He asks what they eat, learns their favorite foods, and finds out if foods that he deems important for the gut-brain connection are missing from their diets, such as plants, seafood and fermented foods.
Dr. Ramsey published a book in March, “ Eat to Beat Depression and Anxiety ,” and founded the Brain Food Clinic in New York to help people struggling with mood disorders improve their diets. He often recites a jingle so people can remember the basics of his dietary advice: “Seafood, greens, nuts and beans — and a little dark chocolate.”
Dr. Ramsey said these foods help to promote compounds like brain-derived neurotrophic factor, or BDNF, a protein that stimulates the growth of new neurons and helps protect existing ones. They also contain large amounts of fiber, unsaturated fat, antioxidants, omega-3 fatty acids and other nutrients that have been shown to improve gut and metabolic health and reduce inflammation, all of which can affect the brain.
Dr. Ramsey said he does not want people to think that the only factor involved in brain health is food. “Lots of people get their food exactly right, live very active lives, and still have significant troubles with their mental health,” he said.
But he also teaches people that food can be empowering. “We can’t control our genes, who our parents were, or if random acts of trauma or violence happen to us,” he said. “But we can control how we eat, and that gives people actionable things that they can do to take care of their brain health on a daily basis.”
Anahad O’Connor is a staff reporter covering health, science, nutrition and other topics. He is also a bestselling author of consumer health books such as “Never Shower in a Thunderstorm” and “The 10 Things You Need to Eat.” More about Anahad O’Connor
How to Be Happy
Happiness can predict health and longevity, but it doesn’t just happen to you..
Small changes in your behavior and surroundings can set you on course for happiness. Here ’s how .
Our seven-day Happiness Challenge will help you focus on a crucial element of living a good life — your relationships .
Finland has been ranked the happiest country on earth for six consecutive years. What’s the secret? The answer is complicated .
Cultivating a sense of wonder can be a salve for a turbulent mind. Here is how to make it part of your everyday life .
It can seem impossible to be optimistic about the future. But these questions will help you understand what all optimists have in common.
Exercise, even in small doses, can improve your mood. Try our eight-minute routine that's based on movements researchers say are inspired by joy.
Advertisement
Food and Mood: the Corresponsive Effect
- Nutrition and the Brain (J Nasser, Section Editor)
- Published: 04 July 2020
- Volume 9 , pages 296–308, ( 2020 )
Cite this article

- Welayah A. AlAmmar 1 ,
- Fatima H. Albeesh 1 &
- Rabie Y. Khattab ORCID: orcid.org/0000-0002-1715-970X 1
6248 Accesses
21 Citations
14 Altmetric
Explore all metrics
Purpose of Review
The question whether food choice and eating behavior influence the mood or are influenced by the mood has been inquisitive to scientists and researchers. The purpose of this review is to support or refuse the argument that mood is affected by food or vice versa.
Recent Findings
The association between food and mood has been comprehensively elucidated in this review based on several studies that include participants from different ages, cultural backgrounds, and health status. The correlation among food, mood, and diseases such as diabetes mellitus, obesity, and depression was thoroughly investigated. The effect of different foods and nutrients on the mood was further explained. It is concluded that the mood significantly affects food intake and food choices. On the other hand, food also influences the mood, which affects the diseases either positively or negatively.
Appropriate food choices play a significant role in mood enhancement. Advertisement is another crucial factor that negatively affects food choices and mood and contributes to many diseases. Understanding the interaction between food and mood can help to prevent or alleviate undesired health issues.
This is a preview of subscription content, log in via an institution to check access.
Access this article
Price includes VAT (Russian Federation)
Instant access to the full article PDF.
Rent this article via DeepDyve
Institutional subscriptions
Similar content being viewed by others

Evidence-based European recommendations for the dietary management of diabetes

Risk factors for eating disorders: findings from a rapid review

An update on the prevalence of eating disorders in the general population: a systematic review and meta-analysis
Papers of particular interest, published recently, have been highlighted as: • of importance •• of major importance.
Liu X, Yan Y, Li F, Zhang D. Fruit and vegetable consumption and the risk of depression: a meta-analysis. Nutrition. 2016;32:296–302. https://doi.org/10.1016/j.nut.2015.09.009 .
Article CAS PubMed Google Scholar
Boddy L, Abayomi J, Johnson B, Hackett A, Stratton G. Ten-year changes in positive and negative marker food, fruit, vegetables, and salad intake in 9-10 year olds: SportsLinx 2000-2001 to 2010-2011. J Hum Nutr Diet. 2013;27:236–41.
PubMed Google Scholar
de la Fuente-Arrillaga C, Zazpe I, Santiago S, Bes-Rastrollo M, Ruiz-Canela M, Gea A, et al. Beneficial changes in food consumption and nutrient intake after 10 years of follow-up in a Mediterranean cohort: the SUN project. BMC Public Health. 2016;16:203. https://doi.org/10.1186/s12889-016-2739-0 .
Article PubMed PubMed Central Google Scholar
James P, Seward M, James OA, Subramanian S, Block J. Changes in the food environment over time: examining 40 years of data in the Framingham Heart Study. Int J Behav Nutr Phys Act. 2017;14:84. https://doi.org/10.1186/s12966-017-0537-4 .
Rooney C, McKinley MC, Woodside JV. The potential role of fruit and vegetables in aspects of psychological well-being: a review of the literature and future directions. P Nutr Soc. 2013;72:420–32.
Google Scholar
Conner T, Brookie K, Carr A, Mainvil L, Vissers M. Let them eat fruit! The effect of fruit and vegetable consumption on psychological well-being in young adults: a randomized controlled trial. PLOS ONE. 2017;12:e0171206. https://doi.org/10.1371/journal.pone.0171206 .
Article CAS PubMed PubMed Central Google Scholar
Mujcic R, Oswald AJ. Evolution of well-being and happiness after increases in consumption of fruit and vegetables. Am J Public Health. 2016;106:1504–10.
PubMed PubMed Central Google Scholar
Raghunathan R, Naylor RW, Hoyer WD. The Unhealthy = Tasty Intuition and Its Effects on Taste Inferences, Enjoyment, and Choice of Food Products. J Mark. 2006;70:170–84.
Evers C, Stok FM, de Ridder DT. Feeding your feelings: emotion regulation strategies and emotional eating. Pers Soc Psychol Bull. 2010;36:792–804.
Wansink B, Cheney MM, Chan N. Exploring comfort food preferences across age and gender. Physiol Behav. 2003;79:739–47.
CAS PubMed Google Scholar
Taut D, Renner B, Baban A. Reappraise the situation but express your emotions: impact of emotion regulation strategies on ad libitum food intake. Front Psychol. 2012;3:359. https://doi.org/10.3389/fpsyg.2012.00359 .
Sproesser G, Schupp HT, Renner B. The bright side of stress-induced eating: eating more when stressed but less when pleased. Psychol Sci. 2013;25:58–65.
Tomiyama JA, Finch LE, Cummings JR. Did that brownie do its job? Stress, eating, and the biobehavioral effects of comfort food. Emerging Trends in the Social and Behavioral Sciences: An Interdisciplinary, Searchable, and Linkable Resource 2015. https://doi.org/10.1002/9781118900772.etrds0324 .
Wagner HS, Ahlstrom B, Redden JP, Vickers Z, Mann T. The myth of comfort food. Health Psychol. 2014;33:1552–7.
Blanchflower DG, Oswald AJ, Stewart-Brown S. Is psychological well-being linked to the consumption of fruit and vegetables? Soc Indic Res. 2013;114:785–801.
White BA, Horwath CC, Conner TS. Many apples a day keep the blues away – daily experiences of negative and positive affect and food consumption in young adults. Br J Health Psychol. 2013;18:782–98.
Schüz B, Bower J, Ferguson SG. Stimulus control and affect in dietary behaviours. An intensive longitudinal study. Appetite. 2015;87:310–7.
•• Wahl D, Villinger K, König L, Ziesemer K, Schupp H, Renner B. Healthy food choices are happy food choices: evidence from a real life sample using smartphone based assessments. Sci Rep. 2017;7:17069. https://doi.org/10.1038/s41598-017-17262-9 This study investigated in-the-moment eating happiness by evaluating complete 8-days real life dietary behavior using smartphone-based momentary assessment tool. The results showed that vegetables consumption contributed the largest share to eating happiness followed by sweets and snacking.
El Ansari W, Suominen S, Berg-Beckhoff G. Mood and food at the University of Turku in Finland: nutritional correlates of perceived stress are most pronounced among overweight students. Int J Public Health. 2015;60:707–16.
Pribis P. Effects of walnut consumption on mood in young adults—a randomized controlled trial. Nutrients. 2016;8:668. https://doi.org/10.3390/nu8110668 .
Article CAS PubMed Central Google Scholar
Parker G, Brotchie H. Mood effects of the amino acids tryptophan and tyrosine. Acta Psychiatr Scand. 2011;124:417–26.
Kroes M, van Wingen G, Wittwer J, Mohajeri M, Kloek J, Fernández G. Food can lift mood by affecting mood-regulating neurocircuits via a serotonergic mechanism. Neuroimage. 2014;84:825–32.
Collins R, Stafford L. Feeling happy and thinking about food. Counteractive effects of mood and memory on food consumption. Appetite. 2015;84:107–12.
Christensen L. The effect of food intake on mood. Clin Nutr. 2001;20:161–6.
CAS Google Scholar
Bongers P, Jansen A, Havermans R, Roefs A, Nederkoorn C. Happy eating. The underestimated role of overeating in a positive mood. Appetite. 2013;67:74–80.
Hendy H. Which comes first in food–mood relationships, foods or moods? Appetite. 2012;58:771–5.
England C, Thompson J, Jago R, Cooper A, Andrews R. Development of a brief, reliable and valid diet assessment tool for impaired glucose tolerance and diabetes: the UK Diabetes and Diet Questionnaire. Public Health Nutr. 2016;20:191–9.
Hood M, Reutrakul S, Crowley S. Night eating in patients with type 2 diabetes. Associations with glycemic control, eating patterns, sleep, and mood. Appetite. 2014;79:91–6.
Raymond K, Lovell G. Food addiction symptomology, impulsivity, mood, and body mass index in people with type two diabetes. Appetite. 2015;95:383–9.
TODAY Study Group, Wilfley D, Berkowitz R, et al. Binge eating, mood, and quality of life in youth with type 2 diabetes: baseline data from the TODAY study. Diabetes Care. 2011;34:858–60.
Alfonso-Rosa R, del Pozo-Cruz B, Del Pozo-Cruz J, Del Pozo-Cruz J, Sañudo B. The relationship between nutritional status, functional capacity, and health-related quality of life in older adults with type 2 diabetes: a pilot explanatory study. J Nutr Health Aging. 2013;17:315–21.
• Gibson-Smith D, Bot M, Snijder M, et al. The relation between obesity and depressed mood in a multi-ethnic population. The HELIUS study. Soc Psychiatry Psychiatr Epidemiol. 2018;53:629–38 This research examined the relationship between obesity and depressed mood in a large multi-ethnic population. Obesity varied substantially among different ethnic groups, and was associated with a higher risk of depressed mood.
Heo M, Pietrobelli A, Fontaine K, Sirey J, Faith M. Depressive mood and obesity in US adults: comparison and moderation by sex, age, and race. Int J Obes. 2006;30:513–9.
Ladwig K, Marten-Mittag B, Löwel H, Döring A, Wichmann H. Synergistic effects of depressed mood and obesity on long-term cardiovascular risks in 1510 obese men and women: results from the MONICA–KORA Augsburg Cohort Study 1984–1998. Int J Obes. 2006;30:1408–14.
• Privitera G, King-Shepard Q, Cuifolo K, Doraiswamy P. Differential food intake and food choice by depression and body mass index levels following a mood manipulation in a buffet-style setting. J Health Psychol. 2019;24:199–208 This study investigated the effect of different emotional cues on the depression and unhealthy food intake. Obese and depressed participants had significantly greater energy intake following the sad versus happy article reading, due to increased intake of high-calorie foods. These results corroborate recent theories on emotional eating and extend the ecological validity of such effects in a buffet-style setting.
Rose M, Nadler E, Mackey E. Impulse control in negative mood states, emotional eating, and food addiction are associated with lower quality of life in adolescents with severe obesity. J Pediatr Psychol. 2018;43:443–51.
Iyer K, Khan Z. Depression – A Review. Res J Recent Sci. 2012;1:79–87.
Nestler EJ. Epigenetics: stress makes its molecular mark. Nature. 2012;490:171–2.
CAS PubMed PubMed Central Google Scholar
• Larrieu T, Layé S. Food for mood: relevance of nutritional omega-3 fatty acids for depression and anxiety. Front Physiol. 2018;9:1047. https://doi.org/10.3389/fphys.2018.01047 This review addressed the importance of ω3 PUFAs in the prevention and/or treatment of depression and anxiety. Recent experimental studies highlighting how ω3 PUFAs can moderate neurobiological processes involved in anxiety and depression have been covered. Potential mechanisms involved in the neuroprotective and corrective activity of ω3 PUFAs in the brain have been discussed.
Macht M. How emotions affect eating: A five-way model. Appetite. 2008;50:1–11.
Prinz N, Ebner S, Grünerbel A, Henkelüdecke U, Hermanns N, Hummel M, et al. Female sex, young age, northern German residence, hypoglycemia and disabling diabetes complications are associated with depressed mood in the WHO-5 questionnaire – a multicenter DPV study among 17,563 adult patients with type 2 diabetes. J Affect Disord. 2017;208:384–91.
Kotchen T. Obesity-related hypertension: epidemiology, pathophysiology, and clinical management. Am J Hypertens. 2010;23:1170–8.
Singh M. Mood, food, and obesity. Front Psychol. 2014;5:925. https://doi.org/10.3389/fpsyg.2014.00925 .
Kloiber S, Ising M, Reppermund S, Horstmann S, Dose T, Majer M, et al. Overweight and obesity affect treatment response in major depression. Biol Psychiatry. 2007;62:321–6.
Duarte CS, Sourander A, Nikolakaros G, Pihlajamaki H, Helenius H, Piha J, et al. Child mental health problems and obesity in early adulthood. J Pediatr. 2010;156:93–7.
Zhao G, Ford ES, Li C, Tsai J, Dhingra S, Balluz LS. Waist circumference, abdominal obesity, and depression among overweight and obese U.S. adults: National Health and Nutrition Examination Survey 2005-2006. BMC Psychiatry. 2011;11:130. https://doi.org/10.1186/1471-244X-11-130 .
Hamer M, Batty GD, Kivimaki M. Risk of future depression in people who are obese but metabolically healthy: the English longitudinal study of ageing. Mol Psychiatry. 2012;17:940–5.
Fraser LK, Clarke GP, Cade JE, Edwards KL. Fast food and obesity: a spatial analysis in a large United Kingdom population of children aged 13-15. Am J Prev Med. 2012;42e:77–85.
Konttinen H, Männistö S, Sarlio-Lähteenkorva S, Silventoinen K, Haukkala A. Emotional eating, depressive symptoms and self-reported food consumption. A population-based study. Appetite. 2010;54:473–9.
Frank S, Laharnar N, Kullmann S, Veit R, Canova C, Hegner YL, et al. Processing of food pictures: influence of hunger, gender and calorie content. Brain Research. 2010;1350:159–66.
•• Privitera G, Welling D, Tejada G, et al. No calorie comfort: viewing and drawing “comfort foods” similarly augment positive mood for those with depression. J Health Psychol. 2018;23:598–607 This study checked if viewing/drawing visual images of comfort foods in the absence of eating will increase positive mood. Participants viewed/drew foods high or low in fat/sugar; pre-post mood was recorded. Viewing/drawing comfort foods enhanced the mood for those with clinical symptoms of depression. These findings corroborate previous data and reveal a novel finding of augmented mood increases for those with clinical symptoms.
Alpert J, Fava M. Nutrition and depression: the role of folate. Nutr Rev. 1997;55:145–9.
Li Y, Dai Q, Ekperi L, Dehal A, Zhang J. Fish consumption and severely depressed mood, findings from the first national nutrition follow-up study. Psychiatry Res. 2011;190:103–9.
Yeum T, Maggiolo N, Gupta C, Davis B, Nierenberg A, Sylvia L. Adjunctive nutrition therapy for depression. Psychiatr Ann. 2019;49:21–5.
Rogers PJ. Food, mood and appetite. Nutr Res Rev. 95(8):243–69.
Souissi M, Abedelmalek S, Chtourou H, Atheymen R, Hakim A, Sahnoun Z. Effects of morning caffeine’ ingestion on mood states, simple reaction time, and short-term maximal performance on elite judoists. Asian J Sports Med. 2012;3:161–8.
Haskell C, Kennedy D, Wesnes K, Scholey A. Cognitive and mood improvements of caffeine in habitual consumers and habitual non-consumers of caffeine. Psychopharmacology. 2005;179:813–25.
Brice C, Smith A. Effects of caffeine on mood and performance: a study of realistic consumption. Psychopharmacology. 2002;164:188–92.
Lucas M, Mirzaei F, Pan A, Okereke OI, Willett WC, O’Reilly EJ, et al. Coffee, caffeine, and risk of depression among women. Arch Intern Med. 2011;171:1571–8.
Rogers P. Caffeine, mood and mental performance in everyday life. Nutr Bull. 2007;32(s1):84–9.
James J, Gregg M. Effects of dietary caffeine on mood when rested and sleep restricted. Hum Psychopharm Clin. 2004;19:333–41.
Malone R, Giles K, Maloney N, Fyfe C, Lorenzo-Arribas A, O'Connor D, et al. Effects of stress and mood on caffeine consumption in shift and non-shift workers. P Nutr Soc. 2015;74(OCE1):E135. https://doi.org/10.1017/S0029665115001500 .
Article Google Scholar
Cartwright F, Stritzke WG, Durkin K, Houghton S, Burke V, Beilin LJ. Chocolate craving among children: implications for disordered eating patterns. Appetite. 2007;48:87–95.
Fletcher BC, Pine KJ, Woodbridge Z, Nash A. How visual images of chocolate affect the craving and guilt of female dieters. Appetite. 2007;48:211–7.
Meier B, Noll S, Molokwu O. The sweet life: The effect of mindful chocolate consumption on mood. Appetite. 2017;108:21–7.
Ottley C. Food and mood. Nurs Stand. 2000;15:46–52.
Parker G, Parker I, Brotchie H. Mood state effects of chocolate. J Affect Disord. 2006;92:149–59.
Appleton K, McKeown P, Woodside J. Chocolate, biscuits and fruit bars: effects on appetite and mood. P Nutr Soc. 2011;70(OCE3):E106. https://doi.org/10.1017/S0029665111001467 .
Radin D, Hayssen G, Walsh J. Effects of intentionally enhanced chocolate on mood. Explore. 2007;3:485–92.
Kampov-Polevoy A, Alterman A, Khalitov E, Garbutt J. Sweet preference predicts mood altering effect of and impaired control over eating sweet foods. Eating Behav. 2006;7:181–7.
Moreno-Dominguez S, Rodríguez-Ruiz S, Martín M, Warren C. Experimental effects of chocolate deprivation on cravings, mood, and consumption in high and low chocolate-cravers. Appetite. 2012;58:111–6.
Turner S, Luszczynska A, Warner L, Schwarzer R. Emotional and uncontrolled eating styles and chocolate chip cookie consumption. a controlled trial of the effects of positive mood enhancement. Appetite. 2010;54:143–9.
Wolfe A, Arroyo C, Tedders S, Li Y, Dai Q, Zhang J. Dietary protein and protein-rich food in relation to severely depressed mood: a 10 year follow-up of a national cohort. Prog Neuropsychopharmacol Biol Psychiatry. 2011;35:232–8.
Leidy H, Todd C, Zino A, Immel J, Mukherjea R, Shafer R, et al. Consuming high-protein soy snacks affects appetite control, satiety, and diet quality in young people and influences select aspects of mood and cognition. J Nutr. 2015;145:1614–22.
Young H, Benton D, Carter N. The effect of chicken extract on mood, cognition and heart rate variability. Nutrients. 2015;7:887–904.
Baines S, Powers J, Brown WJ. How does the health and well-being of young Australian vegetarian and semi-vegetarian women compare with non-vegetarians? Public health Nutr. 2007;10:436–42.
Jacka F, Pasco J, Williams L, et al. Red meat consumption and mood and anxiety disorders. Psychother Psychosom. 2012;81:196–8.
Larsson CL, Klock KS, Nordrehaug AA, et al. Lifestyle-related characteristics of young low-meat consumers and omnivores in Sweden and Norway. J Adolesc Health. 2002;31:190–8.
Beezhold B, Johnston C. Restriction of meat, fish, and poultry in omnivores improves mood: a pilot randomized controlled trial. Nutr J. 2012;11:9. https://doi.org/10.1186/1475-2891-11-9 .
Ness A, Gallacher J, Bennett P, Gunnell D, Rogers P, Kessler D, et al. Advice to eat fish and mood: a randomised controlled trial in men with angina. Nutr Neurosci. 2003;6:63–5.
Brookie K, Best G, Conner T. Intake of raw fruits and vegetables is associated with better mental health than intake of processed fruits and vegetables. Front Psychol. 2018;9:487. https://doi.org/10.3389/fpsyg.2018.00487 .
Mutanen M, Pajari A-M. Vegetables, whole grains, and their derivatives in cancer prevention. Netherlands: Springer; 2011.
Conner T, Brookie K, Richardson A, Polak M. On carrots and curiosity: eating fruit and vegetables is associated with greater flourishing in daily life. Br J Health Psychol. 2014;20:413–27.
Raaijmakers I, Snoek H, Maziya-Dixon B, Achterbosch T. Drivers of vegetable consumption in Urban Nigeria: food choice motives, knowledge, and self-efficacy. Sustainability. 2018;10:4771. https://doi.org/10.3390/su10124771 .
Khalid S, Barfoot K, May G, Lamport D, Reynolds S, Williams C. Effects of acute blueberry flavonoids on mood in children and young adults. Nutrients. 2017;9:158. https://doi.org/10.3390/nu9020158 .
Lustig RH. Fat chance: beating the odds against sugar, processed food, obesity, and disease. CA, USA: Penguin; 2012.
Kato M, Kumasaka M, Ohnuma S, et al. Comparison of barium and arsenic concentrations in well drinking water and in human body samples and a novel remediation system for these elements in well drinking water. PLOS ONE. 2013;8:e66681. https://doi.org/10.1371/journal.pone.0066681 .
Muñoz C, Johnson E, McKenzie A, et al. Habitual total water intake and dimensions of mood in healthy young women. Appetite. 2015;92:81–6.
Pross N, Demazières A, Girard N, et al. Influence of progressive fluid restriction on mood and physiological markers of dehydration in women. Br J Nutr. 2012;109:313–21.
Armstrong L, Ganio M, Casa D, et al. Mild dehydration affects mood in healthy young women. J Nutr. 2011;142:382–8.
Ganio M, Armstrong L, Casa D, et al. Mild dehydration impairs cognitive performance and mood of men. Br J Nut. 2011;106:1535–43.
Pross N, Demazières A, Girard N, Barnouin R, Metzger D, Klein A, et al. Effects of changes in water intake on mood of high and low drinkers. PLOS ONE. 2014;9:e94754. https://doi.org/10.1371/journal.pone.0094754 .
Institute of Medicine. Dietary reference intakes for water, potassium, sodium, chloride, and sulfate. Washington, DC: The National Academies Press; 2005.
Benton D, Donohoe RT. The effects of nutrients on mood. Public Health Nutr. 1999;2:403–9.
Benton D, Haller J, Fordy J. Vitamin supplementation for 1 year improves mood. Neuropsychobiology. 1995;32:98–105.
Benton D, Griffiths R, Haller J. Thiamine supplementation mood and cognitive functioning. Psychopharmacology. 1997;129:66–71.
Reynolds EH. Folic acid, ageing, depression, and dementia. BMJ. 2002;324(7352):1512–5.
Young SN. Folate and depression–a neglected problem. J Psychiatry Neurosci. 2007;32:80–2.
Pan LA, Martin P, Zimmer T, Segreti AM, Kassiff S, McKain BW, et al. Neurometabolic disorders: potentially treatable abnormalities in patients with treatment-refractory depression and suicidal behavior. Am J Psychiatry. 2017;174:42–50.
Conklin SM, Harris JI, Manuck SB, Yao JK, Hibbeln JR, Muldoon MF. Serum omega-3 fatty acids are associated with variation in mood, personality and behavior in hypercholesterolemic community volunteers. Psychiatry Res. 2007;152:1–10.
Stahl LA, Begg DP, Weisinger RS, Sinclair AJ. The role of omega-3 fatty acids in mood disorders. Curr Opin in Invest Dr. 2008;9:57–64.
Parker G, Gibson NA, Brotchie H, Heruc G, Rees AM, Hadzi-Pavlovic D. Omega-3 fatty acids and mood disorders. Am J Psychiatry. 2006;163:969–78.
Pawels EK, Volterrani D. Fatty acid facts, Part I. Essential fatty acids as treatment for depression, or food for mood? Drug News & Perspectives. 2008;21:446–51.
Kang JX, Gleason ED. Omega-3 Fatty acids and hippocampal neurogenesis in depression. CNS Neurol Disord Drug Targets. 2013;12:460–5.
Grosso G, Galvano F, Marventano S, et al. Omega-3 fatty acids and depression: scientific evidence and biological mechanisms. Oxid Med Cell Longev. 2014:Article ID 313570. https://doi.org/10.1155/2014/313570 .
Harris J, Bargh J, Brownell K. Priming effects of television food advertising on eating behavior. Health Psychology. 2009;28:404–13.
Harris JL, Pomeranz JL, Lobstein T, Brownell KD. A crisis in the marketplace: how food marketing contributes to childhood obesity and what can be done. Annu Rev Public Health. 2009;30:211–25.
Chapman K, Nicholas P, Supramaniam R. How much food advertising is there on Australian television? Health Promot Int. 2006;21:172–80.
Maddock S, Hill B. “Bagels and doughnuts … round food for every mood” food advertising discourses. Brit Food J. 2016;118:327–42.
• Wang R, Liaukonyte J, Kaiser H. Does Advertising Content Matter? Impacts of healthy eating and anti-obesity advertising on willingness to pay by consumer body mass index. Agric Econ Res Rev. 2018;47:1–31 This study examined the influence of healthy eating and anti-obesity advertising on the demand for healthy and unhealthy foods and beverages. Among overweight individuals, anti-obesity advertisements were more effective than healthy eating advertisements at reducing the demand for unhealthy items and increasing the demand for healthy items. The magnitude of this effect increased with BMI. Possible policy implications have been discussed based on the results.
WHO (2019). Commission on ending childhood obesity: facts and figures on childhood obesity. Last update: 23 September 2019 11:57 CEST. Accessed at https://www.who.int/end-childhood-obesity/facts/en/ in October 17, 2019.
Federal Trade Commission (2008). Marketing food to children and adolescents. A review of industry expenditures, activities, and self-regulation. Available at: https://www.ftc.gov/reports/marketing-food-children-adolescents-review-industry-expenditures-activities-self-regulation , Accessed October 17, 2019.
Federal Trade Commission (2007). Children’s exposure to TV advertising in 1977 and 2004. Available at: http://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.82.11&rep=rep1&type=pdf , Accessed October 17, 2019.
Harris JL, Graff SK. Protecting young people from junk food advertising: implications of psychological research for first amendment law. Am J Public Health. 2012;102:214–22. https://doi.org/10.2105/AJPH.2011.300328 .
Chou S-Y, Rashad I, Grossman M. Fast-food restaurant advertising on television and its influence on childhood obesity. J Law Econ. 2008;51:599–618.
Harris JL. Priming obesity: direct effects of television food advertising on eating behavior and food preferences (PhD thesis), New Haven, CT: Yale University; 2008.
Andreyeva T, Kelly IR, Harris JL. Exposure to food advertising on television: associations with children's fast food and soft drink consumption and obesity. Econ Hum Biol. 2011;9:221–33.
Download references
Author information
Authors and affiliations.
Clinical Nutrition Department, Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia
Welayah A. AlAmmar, Fatima H. Albeesh & Rabie Y. Khattab
You can also search for this author in PubMed Google Scholar
Contributions
W.A. and F.A. drafted the initial version of the manuscript. R.K. reviewed, evaluated, and analyzed the content and prepared the final version. All authors approved the final version sharing the responsibility for ensuring the manuscript complies with the journal style requirements and terms of consideration.
Corresponding author
Correspondence to Rabie Y. Khattab .
Ethics declarations
Conflict of interest.
Welayah A. AlAmmar, Fatima H. Albeesh, and Rabie Y. Khattab declare they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Nutrition and the Brain
Rights and permissions
Reprints and permissions
About this article
AlAmmar, W.A., Albeesh, F.H. & Khattab, R.Y. Food and Mood: the Corresponsive Effect. Curr Nutr Rep 9 , 296–308 (2020). https://doi.org/10.1007/s13668-020-00331-3
Download citation
Published : 04 July 2020
Issue Date : September 2020
DOI : https://doi.org/10.1007/s13668-020-00331-3
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Mood;Diseases;Healthy choices
- Find a journal
- Publish with us
- Track your research
Frontiers for Young Minds
- Download PDF
Nutrition and Mental Health—How the Food We Eat Can Affect Our Mood

Food is vital for our survival, it gives us energy, helps us grow, and keeps us healthy. But can it also affect our mood? Science says it can. In the past, a great deal of research has explored how food can affect our physical health. Although this is important, exciting research is now exploring how food can influence our mood and our mental health. Mental health conditions, such as depression affect a significant number of people. This makes research into the effects of food and mood crucial, as food may offer a strategy to help prevent people from getting depression and also help them when they already have depression. Although we are not yet able to explain the exact ways in which food may affect our mood, this research has the potential to decrease the number of people who suffer from mental health conditions, such as depression.
What is Depression?
Depression is a type of illness that influences how we feel. It may develop slowly over time with no external cause and, unlike a physical injury or illness, we cannot always see it just by looking at someone. This is because depression affects the parts of the brain that control how we feel. Diseases that affect our feelings, thoughts and behaviors are called mental illnesses, so depression is a type of mental illness.
We all have times when we feel happy or sad. However, for someone with depression, the feelings of sadness or low mood do not go away. Depression is more than just being sad or down, or losing interest in activities that were once enjoyed, and it can affect everyone in a different way—symptoms are often unique to each individual. A person might, for instance, feel tired all the time and not have much energy, or might find it hard to concentrate. A depressed person may have changes in sleep patterns, have feelings of guilt or low self-worth, or even have changes in appetite [ 1 ]. Symptoms can vary in severity, from rather minor depressive symptoms up to something called major depressive disorder (MDD) , which is a diagnosed clinical condition where multiple symptoms may last for a long time.
Depression is an important mental illness to study, because it affects more than 300 million people from all around the world [ 1 ]. It is one of the most common mental health conditions and can affect both men and women [ 1 ]. In fact, it is predicted that depression will be the number one health concern in the world by the year 2030 [ 2 ]. These statistics show just how important it is to find ways to help prevent people from developing depression and to help people who already have depression.
There are currently a number of ways depression can be treated. One method includes taking a variety of medications. Another includes talking to specialists, such as psychologists, who are trained in treating mental health issues. Although these methods can be effective, there are many people who cannot access these treatments because of where they live, their income, the availability of specialists, or stigma and shame [ 1 ]. Even when people do have access to these treatment methods, some people who try them do not recover completely [ 1 , 3 ]. For this reason, it is important to find other ways to help people with depression. For example, the food that we eat is one factor that might influence our mental health and our mood.
What is Nutrition?
There are many different components that make up the food that we eat. These include a range of nutrients and chemicals, such as macro and micronutrients. Macronutrients are nutrients we need a lot of in our diets and they include carbohydrates, proteins, and fats. Micronutrients are nutrients we need in smaller amounts and they include vitamins and minerals. Along with these nutrients, there are many other important components of food including fiber, water, and antioxidants . These components work together to contribute to the healthy functioning of the human body.
The food we eat can give us energy, help us grow, and keep us healthy—but nutrition involves much more than this. The field of nutrition considers whether people can access and afford to buy food, how foods vary across different cultures, and why we choose to eat the foods that we do. In fact, new ideas about the effects of food are being explored all the time. One idea that is of great importance is how the food we eat can affect our mood. It is possible that the components in food, such as vitamins and minerals, can influence depression. It also explores how depression can influence our food choices [ 4 ]. Figure 1 highlights the connections between what we eat and our mental and physical health.
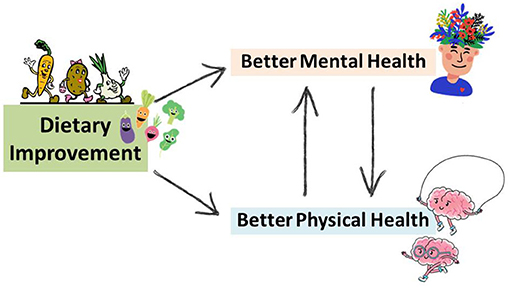
- Figure 1 - Dietary improvement can lead to better mental health and better physical health.
- Mental health and physical health also affect each other.
Food and Mood
Researchers have looked at the connection between diet and depression, and there is now a great deal of evidence suggesting that what we eat every day can influence our mood [ 4 , 5 ]. This research shows that a healthy dietary pattern, such as a Mediterranean-style diet, can have a positive effect on mental health [ 4 , 5 ]. A typical healthy diet pattern is shown in Figure 2 . This includes plenty of vegetables, fruit, nuts, seeds, and olive oil, as well as minimally processed whole grains, legumes, and moderate amounts of lean meat, fish, and dairy. A healthy diet is also low in added sugar and saturated and trans fats , and is high in fiber and antioxidants [ 3 ].
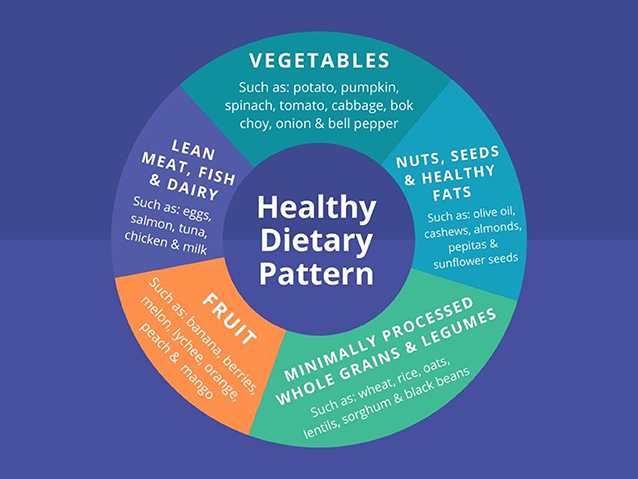
- Figure 2 - A typical healthy dietary pattern includes vegetables, fruit, whole grains, lean meats, dairy, and healthy fats.
Recent studies have explored the link between this healthy dietary pattern and depression. These studies collected information from a large number of people over time. This dietary research has shown a link between unhealthy dietary patterns and symptoms of depression. An unhealthy diet contains mainly ultra-processed foods , including sugar-sweetened beverages, such as soft drinks and packaged snacks that are high in added sugar, salt, and saturated and trans fats. The discovery of this link between diet and depression is important because it suggests that following a healthy dietary pattern over time could possibly prevent depression [ 4 , 5 ].
Other research has shown that a healthy dietary pattern may be able to treat depression. This research looked at the effect of a healthy dietary pattern on people who already had depression. In this Australian study, the researchers compared the results of two different groups of people with depression. Only one group was taught how to follow a healthy dietary pattern. Researchers then looked to see if the changes in their diets improved their mood compared with the group that was not taught to follow a healthy diet. The study showed that people who followed a healthy dietary pattern for 3 months reduced their symptoms of depression [ 5 ].
Why Does Food Help With Depression?
We are not yet able to explain exactly how food may positively affect our mood. However, there are a number of theories as to why this might be the case. Some theories explore the function of different components of food, such as vitamins, minerals, and antioxidants. These theories focus on the role these micronutrients play in contributing to the healthy functioning of the human body. Other theories look at the importance of the microorganisms that live in the gut, called the gut microbiome , and how the foods we eat can affect this microbiome. Lastly, other theories suggest that the changes in behavior that happen when people start to eat a healthy diet may provide the beneficial effects on mood. These behavioral changes could include cooking more at home or cooking and eating in a social setting [ 5 ]. The positive experiences associated with the cultural and social aspect of food may help with depressive symptoms. Remember, nutrition is more than just food giving us energy, keeping us healthy and helping us grow—it is also about foods from different cultures, and why we choose to eat the foods that we do. Therefore, cooking in a social setting may not only influence food choice but may also contribute to a positive food experience and a healthy social environment. Cooking more at home may also help to promote more frequent, healthier food choices.
Finally, there are some studies that look at more specific diets (such as a vegetarian diet) and mental health, but this is not something that has been explored in great detail yet. It would be interesting if more research were done on this subject in the future.
Summary: The Food We Eat Can Affect Our Mood
In conclusion, the food we eat is not only important for our physical health, but also for our mental health. Although more studies are needed to help understand how and why this may be the case, there is now plenty of research that shows what we eat can influence our mood. This suggests diet may be able to play an important role in the prevention and treatment of depression, one of the most common mental health conditions in the world.
Author Contributions
ME drafted the manuscript and approved the final version. JF contributed to the drafting of the manuscript and has approved the final version. JS contributed to the drafting of the manuscript and has approved the final version.
Major Depressive Disorder (MDD) : ↑ A type of depressive disorder, otherwise known as clinical depression, that may be mild, moderate or severe.
Mental Health : ↑ A person’s psychological and emotional well-being.
Antioxidants : ↑ Plant compounds that protect cells from damage.
Nutrition : ↑ The science that looks at the effects of food on the human body.
Trans Fat : ↑ A type of fat that has been shown by researchers to be unhealthy for your heart.
Ultra-processed Foods : ↑ Foods that have been highly manipulated and have ingredients added that are not usually used in cooking, such as artificial colors and flavors.
Gut Microbiome : ↑ The community of different bacteria and microorganisms living in the intestine.
Conflict of Interest
JF is supported by a University of Manchester Presidential Fellowship (P123958) and a UK Research and Innovation Future Leaders Fellowship (MR/T021780/1) and has received support from a NICM-Blackmores Institute Fellowship. JS has received either presentation honoraria, travel support, clinical trial grants, book royalties, or independent consultancy payments from: Integria Healthcare & MediHerb, Pfizer, Scius Health, Key Pharmaceuticals, Taki Mai, FIT-BioCeuticals, Blackmores, Soho-Flordis, Healthworld, HealthEd, HealthMasters, Kantar Consulting, Grunbiotics, Research Reviews, Elsevier, Chaminade University, International Society for Affective Disorders, Complementary Medicines Australia, SPRIM, Terry White Chemists, ANS, Society for Medicinal Plant and Natural Product Research, Sanofi-Aventis, Omega-3 Center, the National Health and Medical Research Council, CR Roper Fellowship.
The remaining author declares that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
[1] ↑ Lim, G. Y., Tam, W. W., Lu, Y., Ho, C. S., Zhang, M. W., and Ho, R. C. 2018. Prevalence of depression in the community from 30 countries between 1994 and 2014. Sci. Rep. 8:2861. doi: 10.1038/s41598-018-21243-x
[2] ↑ World Health Organization. 2008. The Global Burden of Disease: 2004 Update. Geneva: World Health Organization.
[3] ↑ Firth, J., Marx, W., Dash, S., Carney, R., Teasdale, S. B., Solmi, M., et al. 2019. The effects of dietary improvement on symptoms of depression and anxiety: a meta-analysis of randomized controlled trials. Psychosom. Med. 81:265. doi: 10.1097/PSY.0000000000000673
[4] ↑ Sarris, J., Logan, A. C., Akbaraly, T. N., Paul Amminger, G., Balanzá-Martínez, V., Freeman, M. P., et al. 2015. International Society for Nutritional Psychiatry Research consensus position statement: nutritional medicine in modern psychiatry. World Psychiatry . 14:370–1. doi: 10.1002/wps.20223
[5] ↑ Jacka, F. N., O'Neil, A., Opie, R., Itsiopoulos, C., Cotton, S., Mohebbi, M., et al. 2017. A randomised controlled trial of dietary improvement for adults with major depression (the ‘SMILES’ trial). BMC Med .. 15:23. doi: 10.1186/s12916-017-0791-y
- Open access
- Published: 10 November 2023
A scoping review of emotion regulation and inhibition in emotional eating and binge-eating disorder: what about a continuum?
- Mahé Arexis 1 , 2 ,
- Gilles Feron 1 ,
- Marie-Claude Brindisi 1 , 3 ,
- Pierre-Édouard Billot 2 &
- Stéphanie Chambaron 1
Journal of Eating Disorders volume 11 , Article number: 197 ( 2023 ) Cite this article
2669 Accesses
7 Citations
1 Altmetric
Metrics details
Emotional eating is defined as a nonpathological eating behavior, whereas binge-eating disorder (BED) is defined as a pathological eating behavior. While different, both share some striking similarities, such as deficits in emotion regulation and inhibition. Previous research has suggested the existence of an “eating continuum” that might reflect the increased severity of overeating behaviors, that is, from nonpathological overeating to BED. The main aims of this scoping review were to explore in the literature the idea of a continuum between emotional eating and BED and to observe whether deficits in emotion regulation and inhibition follow this continuum in terms of severity. The other aims were to hopefully clarify the ill-defined concept of overeating, to question the potential role of positive emotions and to identify potential knowledge gaps.
A systematic scoping review was conducted following the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) guidelines. Two databases (PubMed/Medline and PsycINFO) were examined in complete accordance with the beforehand sharply defined eligibility and exclusion criteria. The main criteria included adults (≥ 18) with emotional eating, BED or overeating and emotion regulation and inhibition as exposure criteria.
Thirty-two studies were included in this scoping review. If the results showed a link between emotional eating and BED, with the presence of inhibition and emotion regulation deficits in both eating behaviors, no mention of a continuum between emotional eating and BED was found.
In the absence of research directly comparing emotional eating and BED in the same studies and testing the potential increase in severity of emotion regulation and inhibition deficits along this continuum, there is currently no certainty that a continuum exists between emotional eating and BED. In the end, the idea of a continuum in terms of increased severity of overeating and in terms of emotion regulation and inhibition deficits between emotional eating and BED appears to be a gap in knowledge in the literature. This scoping review highlights the need for further research to identify knowledge gaps.
Plain English summary
Emotional eating (EE) is defined as a nonpathological eating behavior, whereas binge-eating disorder (BED) is defined as a pathological eating behavior. While different, both share some striking similarities, such as deficits in emotion regulation (ER) and inhibition. Previous research has suggested the existence of an “eating continuum” that might reflect the increased severity of overeating behaviors, that is, from nonpathological overeating to BED. The main aims of this scoping review were to explore in the literature the idea of a continuum between EE and BED and to observe whether deficits in ER and inhibition follow this continuum in terms of severity. A systematic scoping review was conducted, and thirty-two studies were included in this review. If the results showed a link between EE and BED, with the presence of inhibition and ER deficits in both eating behaviors, no mention of a continuum between EE and BED, or in relation to a continuum, was found. Thus, in the absence of research directly comparing EE and BED in the same studies and testing the potential increase in severity of ER and inhibition deficits along this continuum, there is currently no certainty about the existence or absence of such a continuum.
Introduction
Our scoping review mainly focused on emotional eating (EE) and binge-eating disorder (BED). EE is an eating behavior that can be defined as “the tendency to overeat in response to negative emotions […]” ([ 1 ], p. 106) but in a nonpathological way. It differs from BED, which was formally indexed in 2013 in the DSM-5 as a discrete eating disorder. BED symptoms include recurrent binge-eating episodes (i.e., eating a larger amount of food than most people do during a discrete period of time, with at least one episode per week for three months), “a sense of lack of control over eating during the episode” and “marked distress regarding binge eating”, but without compensatory behaviors as in anorexia nervosa or bulimia nervosa [ 2 ].
Although different, both EE and BED appear to be affected by deficits in emotion regulation (ER) and inhibition [ 3 , 4 , 5 , 6 , 7 , 8 , 9 , 10 ]. Indeed, both individuals with EE and BED present with overeating behaviors caused by emotion regulation difficulties and a lack of inhibition/greater impulsivity. For example, it has been shown that negative emotions act as a trigger for binge-eating episodes in BED [ 7 , 11 , 12 ], and some data also suggest that positive emotions may increase food consumption [ 7 ]. Binge eating can be seen as a way to regulate negative emotions (but it is yet uncertain if this strategy successfully improves mood, see Leehr et al. and Stein et al. [ 7 , 13 ]), and BED patients are more prone to use maladaptive strategies such as suppression or rumination [ 4 ].
Davis [ 14 ] suggested the existence of an “(over) eating continuum”: in some way, on one end of the continuum are nonpathological overeating behaviors and at the other end is BED, which is a pathological and extreme state of overeating. The evolution on this continuum, therefore, reflects the “increased severity and compulsiveness” of overeating behaviors. It is also important to emphasize that this idea of a continuum in severity and compulsiveness between those eating behaviors is also reported by clinicians and physicians. It is therefore reasonable to think that the severity of ER and inhibition deficits could increase along this continuum between EE and BED, as shown in Fig. 1 . Taken together, this information is a starting point to lead a systematic screening of the literature. Since our main goals are to clarify the concept of continuum and to identify knowledge gaps, we chose to conduct a scoping review following the guidelines of PRISMA-ScR (Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews) [ 15 ].
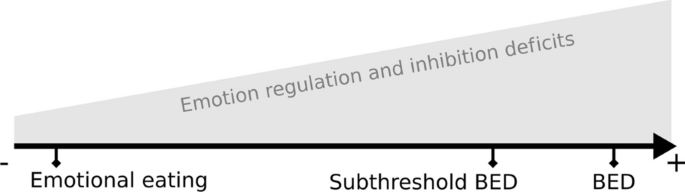
Schematic view of increased emotion regulation and inhibition deficits along a continuum between nonpathological emotional eating and binge-eating disorder (BED)
The present scoping review aimed (1) to address the possible existence of a continuum between EE and BED; (2) to address the possibility of an increase in the severity of deficits in emotion regulation and inhibition; and (3) to address the ill-defined concept of overeating. Indeed, is overeating (OE) a symptom, an eating behavior, a synonymous concept of EE, or a synonym for binge eating? (4) The final aim was to potentially investigate whether positive emotions can, like negative emotions, trigger emotional eating episodes associated with emotion regulation and/or inhibition difficulties. Finally, this scoping review also aimed to identify gaps in knowledge.
The scoping review was conducted following the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) guidelines [ 15 ].
The review protocol can be accessed at HAL ( https://hal.science/hal-03643357v1 —HAL Id/Registration number: hal-03643357) [ 16 ].
Eligibility criteria
Studies were selected based on the following criteria:
The PICOS framework was used to highlight the main criteria. PICOS criteria: Populations : People (adult human subjects ≥ 18) with binge-eating disorder (BED) (and meeting the full DSM-IV-TR or DSM-5 criteria for BED) or subthreshold BED and people (adult human subjects, 18 +) presenting with emotional eating (EE) or emotional overeating (EO). Interventions/Exposures : Our review focused on the impact of “emotion regulation” and “inhibitory control” on BED and EE. Comparisons : Our review did not focus on studies with specific comparisons. Outcomes : Our review considered all types of outcomes related to emotion regulation and inhibitory control in BED, EE, and EO ( e.g. , deficit, level of attention, response impairment, and degree of compulsivity). Studies : All types of journal articles published in peer-reviewed scientific journals, either written in English or in French. The exclusion criteria were all types of reviews, book chapters, abstracts, preprints, theses, and articles focusing on therapies/treatments.
Only papers published between January 2009 and January 2022 were eligible for consideration. Although the MeSH (Medical Subject Headings) terms for binge-eating disorder were not introduced until 2010, the year 2009 was chosen because it was a “transition year” between the previous indexing of binge-eating disorder as bulimia nervosa and the introduction of the MeSH term BED in 2010.
Information sources and search
Two electronic bibliographic databases, PubMed/Medline and PsycINFO, were searched to identify references related to the scoping review topic. The search focused on articles published between January 2009 and January 2022. The following search equation was used in both databases: ("Binge-Eating Disorder"[Mesh] OR BED OR Binge eater OR Emotional Eating OR Emotional Overeating OR Overeater OR Emotional eater OR Overeating) AND ("Emotional Regulation"[Mesh] OR Emotion regulation OR Reappraisal OR Rumination OR Attentional deployment OR Mood regulation OR "Inhibition, Psychological"[Mesh] OR Inhibitory control).
This database search stage was conducted by one of the authors, M. A. No additional references were added from other sources at this stage.
Selection of sources of evidence
Duplicates were removed, and all references were imported into Rayyan, an online application for systematic reviews [ 17 ]. Figure 2 shows the flowchart of the literature search and screening/study selection process. During the successive screening stages, at least 2 authors (M. A., and P.-E. B. or S. C., up to 4 authors, M. A., P.-E. B., S. C. and M.-C. B.) screened each record. Disagreements regarding study selection were resolved by a third or even a fourth investigator, and discussions took place between the authors. In the first screening step, for each article, the inclusion criteria described in Sect. " Eligibility criteria " were applied to both titles and abstracts. In the second screening step (eligibility), for each article, the inclusion criteria described in Sect. " Eligibility criteria " were applied to the entire article (i.e., a complete reading of the article). Note that at this stage, we screened the bibliographic references of the included articles to identify potential new references. At the end of this screening, no new articles were included.
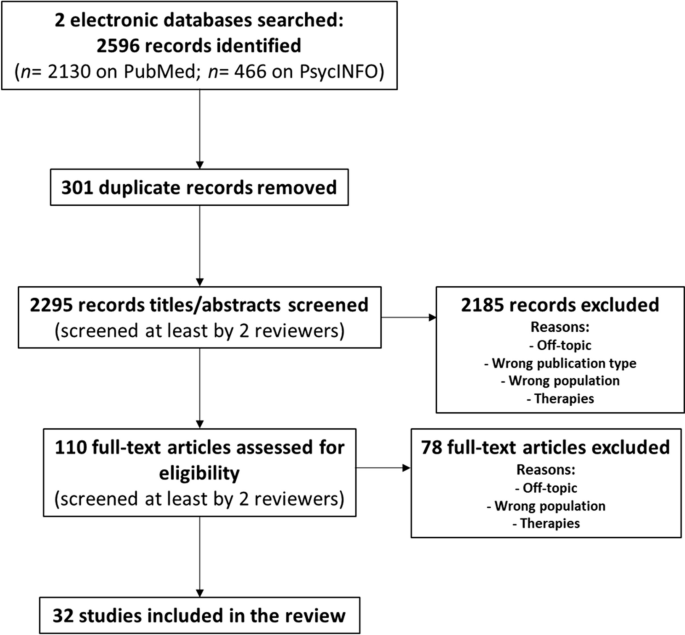
Flowchart of the literature search and screening/study selection process
Data charting process and data items
Three investigators (authors M. A., P.-E. B., and S. C.) developed a data charting form to extract the relevant data from each of the 32 included studies. For each study, author M. A. extracted the data according to the following variables of the chart: authors, title, year of publication, country of the study, journal of publication, type of study, method/study design, participants and sample sizes, type of interventions, comparisons, and outcomes/results. Table 1 shows the final version of the chart with the main characteristics of the studies included in the scoping review. We did not include in Table 1 the journal of publication or type of study variables of the chart, as they were deemed irrelevant for this table. Note that we added in Table 1 a new column “Outcomes/Results highlight” with a simplified overview of the results, as well as a “Limitations” column.
Critical analysis
Two authors (M. A. and P.-E. B.) listed the possible limitations of each study. The limitations identified by both authors were retained, and the others were either eliminated or retained after discussion. A third author (S. C.) checked this list, and her comments were considered. The limitations are summarized in the "Limitations" column of Table 1 and are discussed in Sect. " Critical analysis ".
Synthesis of results
Data were analyzed qualitatively. We first grouped the studies by the types of eating behaviors (emotional eating (EE), overeating (OE), and binge-eating disorder (BED)). Then, we addressed each of the topics formulated in our questions/hypotheses.
The source search in the electronic bibliographic databases retrieved 2596 records (2130 on PubMed/Medline and 466 on PsycINFO) (see Fig. 2 ). After removing 301 duplicate records, 2295 records were screened in the first screening step. During this first screening step, for each of the 2295 articles, the inclusion criteria described in the Eligibility criteria section of the Methods section were applied to both titles and abstracts, resulting in 110 records to be assessed for eligibility in the next step. Thus, in the second screening step (eligibility), for each of the 110 articles, the same inclusion criteria were applied to the entire article (i.e., a complete reading of the article). At the end of this second stage, 32 studies were selected to be included in the review. Table 1 shows the main characteristics of the 32 studies included in the scoping review, according to the variables described in Sect. " Data charting process and data items ".
Regarding the types of populations (cf. PICOS criteria), 9 studies out of 32 focused on emotional eating (EE), 21 studies out of 32 focused on binge-eating disorder (BED), and 2 out of 32 focused on overeating (OE). Regarding the types of intervention/exposure (cf. PICOS criteria), namely, ER and inhibition/impulsivity, 19 studies out of 32 focused on emotion regulation (ER), 18 studies out of 32 focused on inhibition/impulsivity, and 5 out of 32 focused on both ER and inhibition/impulsivity. More than a third of the included studies (11 studies out of 32, ≈ 34%) were conducted in Germany. Moreover, more than half of the studies (17 studies out of 32, ≈ 53%) were conducted in Germany or in countries bordering Germany (i.e., France, Switzerland, Belgium and Poland).
Summary of findings
Emotional eating and emotion regulation.
Studies confirm the existence of a link between ER and EE, including the fact that ER difficulties predict EE. For example, Stapleton and Whitehead [ 18 ] highlighted that “Emotion regulation difficulties was the greatest predictor of emotional eating, suggesting that individuals who have difficulty regulating their emotions are more likely to engage in emotional eating behavior”. Similarly, Crockett et al. [ 3 ] concluded that “In every model we tested, difficulties in emotion regulation predicted emotional eating”. Sultson and Akkermann [ 19 ] concluded that "Higher level of ER difficulties among obese and normal weight individuals with EE also lend further support for the assumption that emotion dysregulation might underlie EE". Kornacka et al. [ 20 ] highlighted the “[…] crucial role of ruminative thinking in the occurrence of emotional eating […]”. Regarding avoidance, Deroost and Cserjési [ 21 ] showed “[…] that people with a high degree of EM use avoidance as a primary coping strategy" and added that "avoidance coping also significantly predicted the level of EM” (EM = emotional eating).
Future studies focusing on EE and ER should separately test other specific types of emotional eating (e.g., EE in response to depression, to anxiety…). Indeed, Braden et al. [ 22 ] explained that “exploratory analyses suggest possible unique relationships between types of emotional eating and specific facets of emotion regulation”. The authors added that “[…] findings suggest that certain emotion regulation strategies may be more closely linked to various types of emotional eating”.
Emotional eating and inhibition
The studies included in this scoping review dealing with EE and inhibition/impulsivity confirmed the existence of an association between EE and some inhibition difficulties and impulsivity. For example, Wolz et al. [ 23 ] showed that “[…] emotional eating was not related to general inhibitory control deficits, but was associated with higher behavioral inhibitory control difficulties only while suppressing negative emotions. They added that “[…] the difficulty to inhibit behavioral responses while regulating negative emotions may contribute to disinhibited food intake while experiencing negative emotions”. Stapleton and Whitehead [ 18 ] revealed that emotional eating was related to high impulsivity and that impulsivity was the second greatest predictor of EE after emotion regulation difficulties. Regarding self-control, Wood et al. [ 24 ] showed “[…] an increase in activation across brain regions related to self-control and urges in response to high-calorie food associated with both emotional eating and routine restraint". Taken together, these findings confirm that emotional eaters are prone to inhibition impairments. Moreover, Wolz et al. [ 23 ] suggest that deficits in inhibition only appear when participants are regulating their emotions, highlighting an interesting link between ER and inhibition in EE.
BED and emotion regulation
Concerning BED and emotion regulation, most of the studies confirm the ER difficulties in BED. Leehr et al. [ 25 ] showed that individuals with BED have lower ER capacities. Limited access to ER strategies is also one of the ER difficulties met in BED [ 26 , 27 ], as well as nonacceptance of emotional responses [ 27 ] and lack of emotional clarity [ 26 , 27 ].
BED and inhibition
Overall, studies focusing on BED indicated a deficit in inhibition and increased impulsivity. Leehr et al. [ 25 ] concluded that “Overall, results support the assumption of inhibitory control deficiencies in BED on a behavioral level”. Grant and Chamberlain [ 28 ] underlined that “Binge-eating disorder was associated with impaired response inhibition and executive planning”. Schag et al. [ 29 ] said that “[…] BED represents a neurobehavioural phenotype of obesity that is characterized by increased impulsivity”, and Leehr et al. [ 30 ] showed that “the BED + sample showed higher trait and behavioural impulsivity”. Moreover, according to Aloi et al. [ 31 ], “[…] impaired self-monitoring metacognition and difficulties in impulse control are the central nodes in the psychopathological network of BED […]”.
Overeating and emotion regulation
One of the objectives of this scoping review was to clarify the ill-defined concept of overeating . In the eating disorders literature, overeating sometimes refers to a symptom of an eating disorder or as an eating behavior or is sometimes used as a synonym for emotional eating or binge eating.
Unfortunately, only two of the studies included in this scoping review focused on overeating [ 32 , 33 ], so we could not address this specific question. Nevertheless, similar to EE and BED, those studies highlighted the links between overeating and emotion regulation.
Positive emotions and emotional eating
We questioned the possibility of positive emotions causing emotional eating episodes associated with emotion regulation and/or inhibition difficulties (in the same way as negative emotions). Based on the studies included in our review, opinions differ regarding this point. Indeed, while an article highlights that “[…] positive EE was associated with elevated levels of ER difficulties, suggesting that overeating in response to positive emotions might also include some features of emotion dysregulation” [ 19 ], another article concludes, on the contrary, that “[…] eating in response to positive emotions was not significantly related to poorer psychological well-being, greater eating disorder symptoms, or emotion dysregulation” [ 22 ]. Since there is yet no consensus on the subject, further research on emotional eating needs to be conducted to separately test and dissociate positive and negative emotions.
Positive emotions and BED
We wondered about positive emotions as a possible cause of emotional eating episodes associated with emotion regulation and/or inhibition difficulties. We checked whether the BED studies included in this scoping review addressed the question of positive emotions/affect/mood. Loeber et al. [ 34 ] showed that “[…] restrained eating and mood are factors that moderate response inhibition to food-associated stimuli in obese patients with BED” and that “[…] apart from negative mood, positive mood might as well be a trigger for loss of control over eating behaviour”.
Finally, it is worth mentioning that one study showed that negative and positive mood levels are different during binge days, with an increasing negative mood and a decreasing positive mood at the first binge-eating episode (see Munsch et al. [ 35 ]).
Emotional eating and weight profiles
Studies included in this scoping review tended to show that the relationships between EE and emotion dysregulation (and anxiety, depression, and rumination) might be different according to the weight profile (i.e., normal weight, overweight, and with moderate or severe obesity) (see, for example, Willem et al. [ 36 ] or Kornacka et al. [ 20 ]). Willem et al. [ 36 ] highlighted that “emotion dysregulation, anxiety and depression have different impacts on emotional eating (EE) depending on obesity severity", while Kornacka et al. [ 20 ] underlined that “the role of emotional eating in the link between rumination and uncontrolled eating is different in overweight vs. healthy individuals”.
Emotional eating, BED and rumination
According to three of the studies included in this scoping review, rumination, a maladaptive emotion regulation strategy, is encountered in both EE and BED. Indeed, in EE, Kornacka et al. [ 20 ] highlight that rumination is a predictor of EE (“[…] the results of the two studies confirm the crucial role of ruminative thinking in the occurrence of emotional eating […]”. Similarly, people with BED are more inclined than healthy people to use rumination as a negative emotion regulation strategy [ 27 ]. Wang et al. [ 37 ] also highlighted that “[…] rumination is an important cognitive process associated with severity of eating-disorder psychopathology”.
The idea of a possible continuum
We hypothesized that there would be a continuum between EE (nonpathological eating behavior) and BED (pathological eating behavior). Three studies focusing on BED mentioned this idea of a continuum in the severity of eating disorders. Leehr et al. [ 25 ] stated that “From a clinical perspective eating behavior of the three groups can be seen on a continuum from normal eating behavior, to overeating, to binge eating”. Mobbs et al. [ 38 ] highlighted that “[…] these cognitive deficits are more severe in obese patients with binge eating disorder, which indicates that there is a continuum of increasing inhibition and cognitive problems with increasingly disordered eating”. Moreover, Svaldi et al. [ 39 ] underlined that “[…] the magnitude of the inhibitory deficit was found to be related to the reported severity of eating pathology”, which is compatible with the idea of a continuum.
However, none of the reviewed studies directly compared EE to BED regarding ER or inhibition performances, neither in a longitudinal nor cross-sectional design. Thus, a gap can clearly be identified in this specific field since there is a complete lack of experimental data about an increased severity in ER and inhibition deficit between EE and BED.
We identified some limitations between studies, and some of them were quite redundant in our corpus. First, half of the included studies recorded only self-reported data using scales, questionnaires, or interviews. These declarative measures often suffer from memory bias or social desirability concerns [ 40 ]. Moreover, these measures are often carried out for a particular purpose, and this purpose may differ from study to study, depending on the research question being asked [ 40 ]. Strikingly, 88.9% of papers addressing ER gathered only self-report measures (but only 11.8% for inhibition). Thus, there is a lack of experimental data to address the issue of ER in BED and EE.
Second, 43.8% of the articles with self-report measures only appeared to have rather small sample sizes and/or unbalanced groups and were therefore underpowered. Sample size is a critical issue for quantitative analysis. This sample size must be large enough to achieve the appropriate level of measurement precision. [ 41 ].
Third, most of the participants enrolled in these studies were women, compromising the generalizability to the global population (81.3% of studies had only women participants or an unbalanced sex ratio toward women). Eating disorders are more frequent among women, and for BED, the ratio varies between 1:2 and 1:6 [ 42 ]. Thus, while the lack of men in BED studies is understandable, future studies should consider recruiting more men to properly balance the experimental groups.
Finally, a recurring limitation emphasized by many authors of the included studies is that their research was cross-sectional. Indeed, given the short duration of these types of studies, it was impossible to reveal some causal links between different phenomena (e.g., between BED and impulsivity). However, in our opinion, this is not a limitation per se, as cross-sectional and longitudinal studies are two very different types of research. Therefore, we did not report this limitation in Table 1 .
The main objectives of this scoping review were to explore the idea of a continuum between EE and BED as well as explore the idea of a gradation in emotion regulation and inhibition deficits along this continuum. This hypothesis is supported by some authors and is widely discussed in Davis [ 14 ]. He developed the concept of an “eating continuum”, ranging from homeostatic eating (energy balance) to food addiction, with different levels of “overeating”, including BED-like symptoms and diagnosed BED. It should also be noted that this idea of a continuum is shared by many physicians in their daily clinical practice and that this idea needs to be verified.
The most striking result of our scoping review is that there are strong similarities between EE and BED, with emotional eaters and BED patients sharing the same difficulties in emotion regulation and inhibition. Some of the included studies seem to be compatible with the idea of a gradation of ER and inhibition deficits following this continuum. For instance, Mobbs et al.’s [ 38 ] conclusions strengthened the idea of a continuum of inhibition impairment, with BED patients living with obesity having more difficulties inhibiting their responses compared to controls living with obesity. Indeed, the authors concluded that “[…] these cognitive deficits are more severe in obese patients with binge eating disorder, which indicates that there is a continuum of increasing inhibition and cognitive problems with increasingly disordered eating”. Concerning EE, the results of Sultson and Akkermann [ 19 ] showed that participants with EE have more binge eating behaviors than participants without EE but do not meet all the DSM-5 criteria to be diagnosed with BED. These results suggest that EE could lead to BED and thus support the idea of a continuum. It is, however, crucial to remember that none of the articles included in this review directly compared EE and BED in the same study, neither in a longitudinal nor cross-sectional design. To ascertain the existence of a continuum between EE and BED, the increased severity of ER and inhibition deficits between EE and BED still need to be proven. One of the main goals of this scoping review was also to identify knowledge gaps, and indeed, we found a gap in the literature regarding the increased severity in ER and inhibition impairments from EE to BED. Such a lack of experimental work is truly surprising given the feelings shared by many caregivers in the field of eating disorders as well as the thoughts shared by some authors [ 14 , 25 , 38 , 39 ].
Among the thirty-two articles reviewed, only one focused on the relationship between ER and inhibition in EE. Indeed, Wolz et al. [ 23 ] showed that EE was associated with higher behavioral inhibitory control difficulties only while participants were suppressing negative emotions. This outcome should be taken into account in further studies, since ER and inhibition deficits are often studied separately [ 7 , 43 , 44 ]. Indeed, the direct relationship between ER and inhibition remains poorly studied in BED, as well as in EE, but is an important question to explore the idea of a continuum.
The third objective of this scoping review was to address the ill-defined concept of overeating. Unfortunately, only two studies focused on overeating [ 32 , 33 ], and it is thus difficult to clearly define this concept. For both authors, overeating is not an eating disorder per se since participants were healthy volunteers with no prior diagnosis of an eating disorder. However, in both studies, overeating is measured with questionnaires widely used in medical contexts to assess eating disorders, such as the Eating Disorder Examination-Questionnaire (EDE-Q) or the Binge Eating Scale (BES). Thus, overeating may be seen as pathological eating. Moreover, Racine and Horvath [ 33 ] used the Eating Disorder Diagnostic Scale and the Questionnaire on Eating and Weight Patterns-5 (QEWP-5) to determine experimental groups. Women included in the “overeating” group reported consuming an “unusually large amount of food unaccompanied by loss of control over the past 3 months” on both questionnaires. Thus, this inclusion criterion could be a suitable definition of the concept of overeating, but it must be emphasized that there is too little information to properly define this concept.
The fourth aim of this review was to determine whether positive emotions could trigger emotional eating or binge eating episodes associated with emotion regulation and/or inhibition difficulties. Most of the studies only measured EE and binge eating episodes in response to negative emotions. However, few articles specifically focused on positive mood or emotions. Due to a lack of consensus among studies, it was impossible to strongly conclude that positive emotions can affect eating behaviors. Indeed, some data support this idea [ 19 , 34 ], and others are less affirmative [ 22 , 35 ].
Last, concerning the weight profile, it was not one of the aims of this scoping review, but our results showed that emotion regulation deficits were more severe in obese participants than in normal weight or overweight volunteers. Thus, the weight profile seems to be an important parameter when addressing the question of an increased severity in ER deficits between EE and BED.
Limitations
This scoping review presents some limitations. First, regarding the selection phase, not all relevant studies may have been indexed in the two searched databases (PsycINFO and PubMed/Medline). Second, the examination was based on a list of terms describing emotional eating, binge-eating disorder, emotion regulation and inhibition. The possibility that additional articles would have been identified by adding other terms cannot be completely excluded, although the search was intended to be as extensive as possible. Third, a possible limitation of our scoping review is that we did not mention explicitly in our search equation the terms “positive emotions”. Indeed, given that one of our questions was about the possibility that positive emotions can, like negative emotions, trigger emotional eating episodes, we could have perhaps included it in our search equation. Nevertheless, given that we used the inclusive terms “Emotional Regulation”[Mesh]” and “Emotion regulation”, it is likely that we did not miss some interesting records focusing on positive emotions. Finally, in this review, only studies in French or English were included, which did not allow us to be exhaustive in our conclusions.
Conclusion and further directions
In conclusion, this scoping review fully confirmed the presence of inhibition and emotion regulation deficits in both EE and BED, showing strong similarities between these two eating behaviors. However, the lack of experimental data coming from direct comparisons between EE and BED did not make it possible either to confirm the existence or the absence of a possible continuum between EE and BED or an increased severity in ER and inhibition deficits between EE and BED. Thus, this scoping review helped to identify a knowledge gap, and the question of the existence of a continuum still needs to be addressed in further research.
If such a continuum exists, we think it could greatly impact the clinical care of eating disorders. Indeed, if EE can become BED, early care of emotional eaters becomes essential, and early diagnoses could be made. Additionally, prevention could be improved in emotional eaters and even in the general population to avoid progression to an eating disorder (i.e., subthreshold BED and BED) and could also reduce the risk of developing obesity and its comorbidities often associated with BED. Given the variety of symptoms (psychological and physical), monitoring of emotional eaters could be performed by a multidisciplinary medical team, especially for children and adolescents.
The existence of a continuum between EE and BED could also have implications for eating disorder research. In our view, this could lead to further research to develop more specific screening instruments, such as scales and questionnaires. Such instruments might indeed be helpful to classify emotional eater participants into more relevant experimental groups that take into account the severity of EE. To go even further, one could imagine a new scale that would assess the level of eating behaviors across the entire continuum. Moreover, regarding data analysis, data could be analyzed in a discrete way in addition to group comparisons between EE and BED. Last, if such a continuum was verified, it could guide the focus on future research, especially studies on the etiology of BED, and help to better define the concept of “emotional overeating”.
Moreover, to test the idea of a continuum from a different angle, it could be interesting to see if there is an evolution of some other markers between EE and BED, such as biomarkers. Some of them are well known in BED but remain rather poorly studied in EE. Several fMRI studies have shown that brain activation patterns are different in BED patients, especially in the reward system, which explains why this eating disorder is often associated with food addiction [ 14 ]. For example, the ventral striatum and the medial prefrontal cortex seem to be underactivated during a rewarding task. Moreover, the ventral putamen, orbitofrontal cortex, amygdala, and insula respond less in BED patients than in controls [ 8 ]. EEG studies have also provided a valuable understanding of neurophysiological markers. In their narrative review, Berchio et al. [ 45 ] found that behavioral traits of BED and bulimia nervosa, such as loss of control over eating and emotional eating, are associated with an increased attentional reactivity (P300 wave) to visual food stimuli. Finally, animal studies allow us to better understand the functioning of some molecules. For example, the role of dopamine, oxytocin, and opiate in eating disorders is well understood [ 46 ], and this could be an interesting focus to measure the gradation between EE and BED.
Availability of data and materials
Two electronic bibliographic databases, PubMed/Medline and PsycINFO, were searched to identify references related to the scoping review topic. The search focused on articles published between January 2009 and January 2022. Original records (before screening) can be found using the search equation that was used in both databases: ("Binge-Eating Disorder"[Mesh] OR BED OR Binge eater OR Emotional Eating OR Emotional Overeating OR Overeater OR Emotional eater OR Overeating) AND ("Emotional Regulation"[Mesh] OR Emotion regulation OR Reappraisal OR Rumination OR Attentional deployment OR Mood regulation OR "Inhibition, Psychological"[Mesh] OR Inhibitory control). The 32 articles included after the screening steps are listed in the References section.
Abbreviations
- Emotional eating
- Binge-eating disorder
- Emotion regulation
Preferred reporting items for systematic reviews and meta-analyses extension for scoping reviews
Populations, interventions, comparisons, outcomes, studies
Diagnostic and statistical manual of mental disorders Text Revision, or 5th edition
Electroencephalography
Magnetoencephalography
Normal weight controls
Food stroop task
Body mass index
Barratt impulsiveness scale
Ecological momentary assessment
Bulimia nervosa
Healthy controls
Eating disorders
Difficulties in emotion regulation scale
People living with BED (or subthreshold BED, depending on the studies)
People living without BED (or subthreshold BED, depending on the studies)
Loss of control
Objective binge episode
Late positive potential
Stop signal task
Stop signal reaction time
Functional magnetic resonance imaging
Healthy volunteers
Go-trial reaction time
Normal-weight people living with BED
Overweight people living with BED
Executive functioning
Non-BED obese individuals
Lean comparison
Ventromedial prefrontal cortex
Inferior frontal gyrus
Anorexia nervosa-restricting type
Anorexia nervosa–binge/purge type
Eating disorder, not otherwise specified
Emotional eating/eaters (depending on the studies)
Exogenous cueing task
Network analysis
Emotional overeating
Medical subject headings
Emotional eating (used in some of the included articles)
Eating disorder examination-questionnaire (EDE-Q)
Binge eating scale
Eating disorder diagnostic scale and the questionnaire on eating and weight patterns-5
van Strien T, van de Laar FA, van Leeuwe JFJ, Lucassen PLBJ, van den Hoogen HJM, Rutten GEHM, et al. The dieting dilemma in patients with newly diagnosed type 2 diabetes: does dietary restraint predict weight gain 4 years after diagnosis? Health Psychol. 2007;26(1):105–12.
Article PubMed Google Scholar
American Psychiatric Association. Diagnostic and statistical manual of mental disorders: DSM-5. 5th ed. Washington: American psychiatric association; 2013.
Book Google Scholar
Crockett AC, Myhre SK, Rokke PD. Boredom proneness and emotion regulation predict emotional eating. J Health Psychol. 2015;20(5):670–80.
Dingemans A, Danner U, Parks M. Emotion regulation in binge eating disorder: a review. Nutrients. 2017;9(11):1274.
Article PubMed PubMed Central Google Scholar
Ferrell EL, Watford TS, Braden A. Emotion regulation difficulties and impaired working memory interact to predict boredom emotional eating. Appetite. 2020;144:104450.
Giel KE, Teufel M, Junne F, Zipfel S, Schag K. Food-related impulsivity in obesity and binge eating disorder-a systematic update of the evidence. Nutrients. 2017;9(11):1170.
Leehr EJ, Krohmer K, Schag K, Dresler T, Zipfel S, Giel KE. Emotion regulation model in binge eating disorder and obesity–a systematic review. Neurosci Biobehav Rev. 2015;49:125–34.
Steward T, Menchon JM, Jiménez-Murcia S, Soriano-Mas C, Fernandez-Aranda F. Neural network alterations across eating disorders: a narrative review of fMRI studies. Curr Neuropharmacol. 2018;16(8):1150–63.
Waltmann M, Herzog N, Horstmann A, Deserno L. Loss of control over eating: a systematic review of task based research into impulsive and compulsive processes in binge eating. Neurosci Biobehav Rev. 2021;129:330–50.
Zhang P, Wu GW, Yu FX, Liu Y, Li MY, Wang Z, et al. Abnormal regional neural activity and reorganized neural network in obesity: evidence from resting-state fMRI. Obes Silver Spring Md. 2020;28(7):1283–91.
Article Google Scholar
Greeno CG, Wing RR, Shiffman S. Binge antecedents in obese women with and without binge eating disorder. J Consult Clin Psychol. 2000;68(1):95–102.
Nicholls W, Devonport TJ, Blake M. The association between emotions and eating behaviour in an obese population with binge eating disorder: emotions and binge eating disorder. Obes Rev. 2016;17(1):30–42.
Stein RI, Kenardy J, Wiseman CV, Dounchis JZ, Arnow BA, Wilfley DE. What’s driving the binge in binge eating disorder?: a prospective examination of precursors and consequences. Int J Eat Disord. 2007;40(3):195–203.
Davis C. From passive overeating to « food addiction »: a spectrum of compulsion and severity. ISRN Obes. 2013;2013:435027.
PubMed PubMed Central Google Scholar
Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169(7):467–73.
Arexis M, Feron G, Brindisi MC, Billot PE, Chambaron S. Impacts of emotional regulation and inhibition on Emotional Eating (EE) and Binge Eating Disorder (BED): Protocol for a scoping review. Hal-03643357. 2022.
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A. Rayyan—a web and mobile app for systematic reviews. Syst Rev. 2016;5(1):210.
Stapleton P, Whitehead M. Dysfunctional eating in an Australian community sample: the role of emotion regulation, impulsivity, and reward and punishment sensitivity. Aust Psychol. 2014;49(6):358–68.
Sultson H, Akkermann K. Investigating phenotypes of emotional eating based on weight categories: a latent profile analysis. Int J Eat Disord. 2019;52(9):1024–34.
Kornacka M, Czepczor-Bernat K, Napieralski P, Brytek-Matera A. Rumination, mood, and maladaptive eating behaviors in overweight and healthy populations. Eat Weight Disord EWD. 2021;26(1):273–85.
Deroost N, Cserjési R. Attentional avoidance of emotional information in emotional eating. Psychiatry Res. 2018;269:172–7.
Braden A, Musher-Eizenman D, Watford T, Emley E. Eating when depressed, anxious, bored, or happy: are emotional eating types associated with unique psychological and physical health correlates? Appetite. 2018;125:410–7.
Wolz I, Biehl S, Svaldi J. Emotional reactivity, suppression of emotions and response inhibition in emotional eaters: a multi-method pilot study. Appetite. 2021;161:105142.
Wood SMW, Schembre SM, He Q, Engelmann JM, Ames SL, Bechara A. Emotional eating and routine restraint scores are associated with activity in brain regions involved in urge and self-control. Physiol Behav. 2016;165:405–12.
Leehr EJ, Schag K, Dresler T, Grosse-Wentrup M, Hautzinger M, Fallgatter AJ, et al. Food specific inhibitory control under negative mood in binge-eating disorder: evidence from a multimethod approach. Int J Eat Disord. 2018;51(2):112–23.
Gianini LM, White MA, Masheb RM. Eating pathology, emotion regulation, and emotional overeating in obese adults with Binge Eating Disorder. Eat Behav. 2013;14(3):309–13.
Walenda A, Kostecka B, Santangelo PS, Kucharska K. Examining emotion regulation in binge-eating disorder. Borderline Personal Disord Emot Dysregulation. 2021;8(1):25.
Grant JE, Chamberlain SR. Neurocognitive findings in young adults with binge eating disorder. Int J Psychiatry Clin Pract. 2020;24(1):71–6.
Schag K, Teufel M, Junne F, Preissl H, Hautzinger M, Zipfel S, et al. Impulsivity in binge eating disorder: food cues elicit increased reward responses and disinhibition. PLoS ONE. 2013;8(10):e76542.
Leehr EJ, Schag K, Brückmann C, Plewnia C, Zipfel S, Nieratschker V, et al. A putative association of COMT Val(108/158)met with impulsivity in binge eating disorder. Eur Eat Disord Rev J Eat Disord Assoc. 2016;24(2):169–73.
Aloi M, Rania M, Carbone EA, Caroleo M, Calabrò G, Zaffino P, et al. Metacognition and emotion regulation as treatment targets in binge eating disorder: a network analysis study. J Eat Disord. 2021;9(1):22.
Görlach MG, Kohlmann S, Shedden-Mora M, Rief W, Westermann S. Expressive suppression of emotions and overeating in individuals with overweight and obesity. Eur Eat Disord Rev J Eat Disord Assoc. 2016;24(5):377–82.
Racine SE, Horvath SA. Emotion dysregulation across the spectrum of pathological eating: comparisons among women with binge eating, overeating, and loss of control eating. Eat Disord. 2018;26(1):13–25.
Loeber S, Rustemeier M, Paslakis G, Pietrowsky R, Müller A, Herpertz S. Mood and restrained eating moderate food-associated response inhibition in obese individuals with binge eating disorder. Psychiatry Res. 2018;264:346–53.
Munsch S, Meyer AH, Quartier V, Wilhelm FH. Binge eating in binge eating disorder: a breakdown of emotion regulatory process? Psychiatry Res. 2012;195(3):118–24.
Willem C, Gandolphe MC, Doba K, Roussel M, Verkindt H, Pattou F, et al. Eating in case of emotion dys-regulation, depression and anxiety: different pathways to emotional eating in moderate and severe obesity. Clin Obes. 2020;10(5):e12388.
Wang SB, Lydecker JA, Grilo CM. Rumination in patients with binge-eating disorder and obesity: associations with eating-disorder psychopathology and weight-bias internalization. Eur Eat Disord Rev J Eat Disord Assoc. 2017;25(2):98–103.
Mobbs O, Iglesias K, Golay A, Van der Linden M. Cognitive deficits in obese persons with and without binge eating disorder. Investigation using a mental flexibility task. Appetite. 2011;57(1):263–71.
Svaldi J, Naumann E, Trentowska M, Schmitz F. General and food-specific inhibitory deficits in binge eating disorder. Int J Eat Disord. 2014;47(5):534–42.
Kimberlin CL, Winterstein AG. Validity and reliability of measurement instruments used in research. Am J Health-Syst Pharm AJHP Off J Am Soc Health-Syst Pharm. 2008;65(23):2276–84.
Frost MH, Reeve BB, Liepa AM, Stauffer JW, Hays RD. Mayo/FDA patient-reported outcomes consensus meeting group; What is sufficient evidence for the reliability and validity of patient-reported outcome measures? Value Health J Int Soc Pharmacoeconomics Outcomes Res. 2007;10(Suppl 2):S94-105.
Raevuori A, Keski-Rahkonen A, Hoek HW. A review of eating disorders in males. Curr Opin Psychiatry. 2014;27(6):426–30.
Carr MM, Wiedemann AA, Macdonald-Gagnon G, Potenza MN. Impulsivity and compulsivity in binge eating disorder: a systematic review of behavioral studies. Prog Neuropsychopharmacol Biol Psychiatry. 2021;12:110318.
Saruco E, Pleger B. a systematic review of obesity and binge eating associated impairment of the cognitive inhibition system. Front Nutr. 2021;8:609012.
Berchio C, Cambi S, Pappaianni E, Micali N. EEG biomarkers in children and adolescents with feeding and eating disorders: current evidence and future directions. Front Psychiatry. 2022;13:882358.
Turton R, Chami R, Treasure J. Emotional eating, binge eating and animal models of binge-type eating disorders. Curr Obes Rep. 2017;6(2):217–28.
Download references
Acknowledgements
Not applicable.
This scoping review was supported by grants from the French National Research Agency [Agence Nationale de la Recherche (ANR): ImplicEAT project ANR-17-CE21-0001].
Author information
Authors and affiliations.
Centre Des Sciences du Goût Et de L’Alimentation, CNRS, INRAE, Institut Agro, Université de Bourgogne, 21000, Dijon, France
Mahé Arexis, Gilles Feron, Marie-Claude Brindisi & Stéphanie Chambaron
Université de Franche-Comté, LINC, 25000, Besançon, France
Mahé Arexis & Pierre-Édouard Billot
Centre Spécialisé de L’Obésité Bourgogne, Centre Hospitalier Universitaire Dijon Bourgogne, Dijon, France
Marie-Claude Brindisi
You can also search for this author in PubMed Google Scholar
Contributions
All authors participated in the conception of the study. Three investigators (authors MA, P-EB, and SC) developed a data charting form to extract the relevant data from each of the 32 included studies. For each study, author MA extracted the data according to the following variables of the chart: authors, title, year of publication, country of the study, journal of publication, type of study, method/study design, participants and sample sizes, type of interventions, comparisons, and outcomes/results. Two authors (MA and P-EB) listed the possible limitations of each study. The limitations identified by both authors were retained, and the others were either eliminated or retained after discussion. Two authors (SC and M-CB) checked this list, and their comments were considered. MA wrote the first draft of the article and MA, P-EB, SC and M-CB contributed to the final version. All authors proofread the final version.
Corresponding author
Correspondence to Pierre-Édouard Billot .
Ethics declarations
Ethics approval and consent to participate.
This scoping review did not involve animals or human participants, and we did not use personal information. All data used in this review were extracted from published articles.
Consent for publication
This scoping review did not involve human participants, and we did not use personal information. Thus, consent for publication was unnecessary for this scoping review.
Competing interests
The authors declare that they have no competing interests.
The review protocol can be accessed at HAL ( https://hal.science/hal-03643357v1 —HAL Id/Registration number: hal-03643357). Protocol reference: Arexis, M., Feron, G., Brindisi, M.-C., Billot, P.-E., & Chambaron, S. (2022). Impacts of emotional regulation and inhibition on Emotional Eating (EE) and Binge Eating Disorder (BED): Protocol for a scoping review. Hal-03643357 .
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Arexis, M., Feron, G., Brindisi, MC. et al. A scoping review of emotion regulation and inhibition in emotional eating and binge-eating disorder: what about a continuum?. J Eat Disord 11 , 197 (2023). https://doi.org/10.1186/s40337-023-00916-7
Download citation
Received : 24 February 2023
Accepted : 18 October 2023
Published : 10 November 2023
DOI : https://doi.org/10.1186/s40337-023-00916-7
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Scoping review
Journal of Eating Disorders
ISSN: 2050-2974
- General enquiries: [email protected]
Watch CBS News
Limit these ultra-processed foods for longer-term health, 30-year study suggests
By Sara Moniuszko
Edited By Paula Cohen
Updated on: May 10, 2024 / 11:09 AM EDT / CBS News
New research is adding to the evidence linking ultra-processed foods to health concerns. The study tracked people's habits over 30 years and found those who reported eating more of certain ultra-processed foods had a slightly higher risk of death — with four categories of foods found to be the biggest culprits.
For the study, published in The BMJ , researchers analyzed data on more than 100,000 U.S. adults with no history of cancer, cardiovascular disease or diabetes. Every four years between 1986 and 2018, the participants completed a detailed food questionnaire.
The data showed those who ate the most ultra-processed food — about 7 servings per day — had a 4% higher risk of death by any cause, compared to participants who ate the lowest amount, a median of about 3 servings per day.
Ultra-processed foods include "packaged baked goods and snacks, fizzy drinks, sugary cereals, and ready-to-eat or heat products," a news release for the study noted. "They often contain colors, emulsifiers, flavors, and other additives and are typically high in energy, added sugar, saturated fat, and salt, but lack vitamins and fiber."
Foods with the strongest associations with increased mortality, according to the study, included:
- Ready-to-eat meat, poultry and seafood-based products
- Sugary drinks
- Dairy-based desserts
- Highly processed breakfast foods
Ultra-processed food is a "very mixed group of very different foods," the lead author of the study, Mingyang Song, told CBS News , meaning these categories can offer a helpful distinction.
"Some of the foods actually have really beneficial ingredients like vitamins, minerals, so that's why we always recommend that people not focus too much on the (whole of) ultra-processed food, but rather the individual categories of ultra-processed food."
The research included a large number of participants over a long timespan, but it did have some limitations. As an observational study, no exact cause-and-effect conclusions can be drawn. And the participants were health professionals and predominantly White and non-Hispanic, "limiting the generalizability of our findings," the authors acknowledged.
But they wrote that the findings "provide support for limiting consumption of certain types of ultra-processed food for long term health."
"Future studies are warranted to improve the classification of ultra-processed foods and confirm our findings in other populations," they added.
This study comes after other research published earlier this year found diets high in ultra-processed food are associated with an increased risk of 32 damaging health outcomes , including higher risk for cancer, major heart and lung conditions, gastrointestinal issues, obesity, type 2 diabetes, sleep issues, mental health disorders and early death.
Sara Moniuszko is a health and lifestyle reporter at CBSNews.com. Previously, she wrote for USA Today, where she was selected to help launch the newspaper's wellness vertical. She now covers breaking and trending news for CBS News' HealthWatch.
More from CBS News

Summer 2023 was the hottest in 2,000 years, study finds

Drowning deaths surged during the pandemic — and it was worse among Black people, CDC reports

What is the oldest age for long-term care insurance?

Danish butter magnate's huge coin collection up for sale 100 year's after he died
A surprising solution for reducing our food waste

Every year, we waste 1.3 billion tonnes of food. Here's how that could change. Image: Pexels/Kelly
.chakra .wef-1c7l3mo{-webkit-transition:all 0.15s ease-out;transition:all 0.15s ease-out;cursor:pointer;-webkit-text-decoration:none;text-decoration:none;outline:none;color:inherit;}.chakra .wef-1c7l3mo:hover,.chakra .wef-1c7l3mo[data-hover]{-webkit-text-decoration:underline;text-decoration:underline;}.chakra .wef-1c7l3mo:focus,.chakra .wef-1c7l3mo[data-focus]{box-shadow:0 0 0 3px rgba(168,203,251,0.5);} Cathrine Jansson-Boyd
.chakra .wef-9dduvl{margin-top:16px;margin-bottom:16px;line-height:1.388;font-size:1.25rem;}@media screen and (min-width:56.5rem){.chakra .wef-9dduvl{font-size:1.125rem;}} Explore and monitor how .chakra .wef-15eoq1r{margin-top:16px;margin-bottom:16px;line-height:1.388;font-size:1.25rem;color:#F7DB5E;}@media screen and (min-width:56.5rem){.chakra .wef-15eoq1r{font-size:1.125rem;}} SDG 02: Zero Hunger is affecting economies, industries and global issues

.chakra .wef-1nk5u5d{margin-top:16px;margin-bottom:16px;line-height:1.388;color:#2846F8;font-size:1.25rem;}@media screen and (min-width:56.5rem){.chakra .wef-1nk5u5d{font-size:1.125rem;}} Get involved with our crowdsourced digital platform to deliver impact at scale
Stay up to date:, food insecurity.
- Every year, 1.3 billion tonnes of food is wasted globally, the equivalent of one-third of all food produced for human consumption.
- Busy lives and cooking habits lead to neglecting fresh produce until it spoils, adding to the problem.
- New research finds that keeping a 'food log' for 6 weeks can reduce the amount of waste by an average of 108g per week, an effect that can still be seen six months later.
You’ve had a long day and you’re tired. Faced with making dinner, you look in the fridge and decide to cook something that requires little effort. This is a common scenario, and one that many people act out without really thinking about it.
The fact that there is often little or no conscious thought involved in routine daily food preparation means that ingredients that must be used before they expire are often left to go off.
Two billion people in the world currently suffer from malnutrition and according to some estimates, we need 60% more food to feed the global population by 2050. Yet the agricultural sector is ill-equipped to meet this demand: 700 million of its workers currently live in poverty, and it is already responsible for 70% of the world’s water consumption and 30% of global greenhouse gas emissions.
New technologies could help our food systems become more sustainable and efficient, but unfortunately the agricultural sector has fallen behind other sectors in terms of technology adoption.
Launched in 2018, the Forum’s Innovation with a Purpose Platform is a large-scale partnership that facilitates the adoption of new technologies and other innovations to transform the way we produce, distribute and consume our food.
With research, increasing investments in new agriculture technologies and the integration of local and regional initiatives aimed at enhancing food security, the platform is working with over 50 partner institutions and 1,000 leaders around the world to leverage emerging technologies to make our food systems more sustainable, inclusive and efficient.
Learn more about Innovation with a Purpose's impact and contact us to see how you can get involved.
In research that colleagues and I recently published , we found that overcoming this habitual behaviour is key to cutting food waste. Here’s how to do it.
Every year, 1.3 billion tonnes of food is wasted globally. This is the equivalent of one-third of all the food produced for human consumption.
In the UK alone, households wasted 6.4 million tonnes of food between 2021 and 2022. Accounting for the fossil energy used to grow and harvest that food, as well as the greenhouse gases released when it rots in fields or landfills, this waste equates to 18 million tonnes of CO₂ emissions.
Food waste harms the environment, but reducing how much food is produced only to be thrown away can curb hunger . It could also save the world more than US$120 billion yearly (£96 billion) – and around £700 a year per household.

We measured fruit and vegetable waste from 154 households across the UK for an initial six-week period. Fruit and vegetables are among the most commonly wasted types of food. This may be because supermarkets often sell these ingredients in bulk or because people buying them sometimes fancy something less healthy and more convenient to prepare when the time comes to cook.
During those six weeks, half of the participants were asked to log what fresh fruit and vegetables they bought and when their purchases had to be used according to the label on the packaging, as well as guidelines provided by the researchers.
In each of these homes, the log was placed on the fridge as a daily reminder of what needed to be used each day to avoid waste. Participants also received daily text messages reminding them to check their food log and add any newly bought fruit and vegetables.
The other half of the households involved in this experiment simply measured their food waste at the end of each week without any reminders to use the fresh produce they had.
We expected the half of households receiving reminders to cut their waste more effectively – in fact, there was only a small difference between the two groups. But we did find that simply measuring fresh produce waste made all households more likely to think about what they were wasting.
This was evident from a range of responses from the participants. Taking part in the study also made participants feel as if they could control the amount of food they were throwing away.
It seems that simply asking people to measure their food waste each week for six weeks kickstarts a thinking process that guides people’s behaviour in future.
Food waste on the brain
Our findings may seem obvious, but there is more to them.
We found that across all households the reduction of fresh produce waste averaged 108 grams a week. This was sustained for six months after the experiment ended.
The experience of measuring food waste weekly during the experiment seemed to instil a mindfulness about food waste that meant participants were still throwing less away half a year on. It is interesting that only a short period of conscious effort is necessary to encourage lasting changes in behaviour.

Research into the psychology of food waste tends to focus on nudges, which are subliminal actions to change behaviour, such as menus designed to highlight plant-based options. It is not clear whether such methods, which bypass the conscious mind, work in the long term .
Our study suggests that it takes thought to alter habits. But the good news is that we found people only had to think about reducing food waste for a short time to form an enduring habit of reducing the amount of food they throw away.
Have you read?
7 innovative solutions for fighting food waste, food waste makes up ‘half’ of global food system emissions, could dehydrating meat and vegetables help solve the global food waste problem.
Most people have busy lives and simply don’t have the mental capacity to spare each day. Strategies for reducing food waste that require only a short-term commitment of mental effort are likely to be most effective.
And even a small reduction in household food waste can make a difference. Our study showed that it is relatively easy for people to cut how much fruit and vegetables they discard each week. If just 1,000 people could do the same, it would save over 9.5 tonne of CO₂ a year, the equivalent of 1,140,000 smartphone charges.
Thinking about food waste for six weeks is a small price to pay if the result is a significant and long-term difference to our planet’s wellbeing.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
The Agenda .chakra .wef-n7bacu{margin-top:16px;margin-bottom:16px;line-height:1.388;font-weight:400;} Weekly
A weekly update of the most important issues driving the global agenda
.chakra .wef-1dtnjt5{display:-webkit-box;display:-webkit-flex;display:-ms-flexbox;display:flex;-webkit-align-items:center;-webkit-box-align:center;-ms-flex-align:center;align-items:center;-webkit-flex-wrap:wrap;-ms-flex-wrap:wrap;flex-wrap:wrap;} More on Food and Water .chakra .wef-17xejub{-webkit-flex:1;-ms-flex:1;flex:1;justify-self:stretch;-webkit-align-self:stretch;-ms-flex-item-align:stretch;align-self:stretch;} .chakra .wef-nr1rr4{display:-webkit-inline-box;display:-webkit-inline-flex;display:-ms-inline-flexbox;display:inline-flex;white-space:normal;vertical-align:middle;text-transform:uppercase;font-size:0.75rem;border-radius:0.25rem;font-weight:700;-webkit-align-items:center;-webkit-box-align:center;-ms-flex-align:center;align-items:center;line-height:1.2;-webkit-letter-spacing:1.25px;-moz-letter-spacing:1.25px;-ms-letter-spacing:1.25px;letter-spacing:1.25px;background:none;padding:0px;color:#B3B3B3;-webkit-box-decoration-break:clone;box-decoration-break:clone;-webkit-box-decoration-break:clone;}@media screen and (min-width:37.5rem){.chakra .wef-nr1rr4{font-size:0.875rem;}}@media screen and (min-width:56.5rem){.chakra .wef-nr1rr4{font-size:1rem;}} See all

These are the innovators driving impact in future food systems
Noopur Desai
May 13, 2024

Leveraging technology and innovation to transform food systems
May 6, 2024

These solar-powered sensors can give coffee plants a voice

How to finance the transition to climate-smart agriculture
Greg Goodwin and John Stackhouse
April 29, 2024

How Costa Rica made its seas work for fishermen and for sharks
Diego Vincenzi

From predicting heatwaves to developing climate-resilient seeds: Here’s how agritech can help farmers
Pooja Chhabria and Michelle Meineke
April 28, 2024
- Open access
- Published: 11 May 2024
Natural approach of using nisin and its nanoform as food bio-preservatives against methicillin resistant Staphylococcus aureus and E.coli O157:H7 in yoghurt
- Walaa M. Elsherif 1 , 2 ,
- Alshimaa A. Hassanien 3 ,
- Gamal M. Zayed 2 , 4 &
- Sahar M. Kamal 5
BMC Veterinary Research volume 20 , Article number: 192 ( 2024 ) Cite this article
50 Accesses
Metrics details
Natural antimicrobial agents such as nisin were used to control the growth of foodborne pathogens in dairy products. The current study aimed to examine the inhibitory effect of pure nisin and nisin nanoparticles (nisin NPs) against methicillin resistant Staphylococcus aureus (MRSA) and E.coli O157:H7 during the manufacturing and storage of yoghurt. Nisin NPs were prepared using new, natural, and safe nano-precipitation method by acetic acid. The prepared NPs were characterized using zeta-sizer and transmission electron microscopy (TEM). In addition, the cytotoxicity of nisin NPs on vero cells was assessed using the 3-(4,5-Dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay. The minimum inhibitory concentrations (MICs) of nisin and its nanoparticles were determined using agar well-diffusion method. Further, fresh buffalo’s milk was inoculated with MRSA or E.coli O157:H7 (1 × 10 6 CFU/ml) with the addition of either nisin or nisin NPs, and then the inoculated milk was used for yoghurt making. The organoleptic properties, pH and bacterial load of the obtained yoghurt were evaluated during storage in comparison to control group.
The obtained results showed a strong antibacterial activity of nisin NPs (0.125 mg/mL) against MRSA and E.coli O157:H7 in comparison with control and pure nisin groups. Notably, complete eradication of MRSA and E.coli O157:H7 was observed in yoghurt formulated with nisin NPs after 24 h and 5th day of storage, respectively. The shelf life of yoghurt inoculated with nisin nanoparticles was extended than those manufactured without addition of such nanoparticles.
Conclusions
Overall, the present study indicated that the addition of nisin NPs during processing of yoghurt could be a useful tool for food preservation against MRSA and E.coli O157:H7 in dairy industry.
Peer Review reports

Introduction
Using of bacteriocins such as nisin alone or combined with other natural materials such as essential oils, could be represented as a useful candidate for improving the microbiological quality and maintaining the sensory properties of milk and milk products [ 1 , 2 ]. The utility of nisin as a bio preservative in food industry has been approved and this bacteriocins was effective enough to extended shelf life in regions with inadequate preservation facilities such as developing countries [ 3 ]. Nisin is a natural water-soluble antibacterial peptide (AMP) composed of 34 amino acid residues produced by Lactococcus lactis. It has the ability to inhibit the growth of some foodborne pathogens and many of Gram-positive spoilage bacteria [ 4 , 5 ]. This antibacterial peptide is generally regarded as a safe food preservative by the joint Food and Agriculture Organization and World Health Organization (FAO/WHO), also by the US Food and Drug Administration (FDA) [ 6 , 7 ]. Based on aforementioned permissions, it is widely commercialized as a safe and natural food preservative in the food industry in more than 50 countries around the world [ 8 ].
The antibacterial activity of nisin in food is depending on several factors such as its solubility, pH and structural properties of target bacteria. It could exhibit potent antimicrobial activities against many species of Gram-positive pathogens, while it has little effect against Gram-negative bacteria, yeast and fungi due to their outer membrane barriers [ 9 ]. The exact antibacterial mechanism of nisin is attributed to the passage of nisin through the cell wall of bacteria and its interaction with lipid II, which considered as an essential element in the bacterial cell wall [ 9 ].
There are some obstacles that can hinder the antimicrobial efficacy of free nisin as a food bio preservative such as its ability to interact with food components (e.g. proteolytic enzymes, phospholipids, fatty acids and proteins), high pH and many other food additives. These factors could drastically reduce or completely diminish the antimicrobial effect of nisin [ 10 ]. Hence, different strategies were developed to improve the preservative efficacy of nisin such as liposomes [ 11 ] and nanoparticles [ 12 ]. However, these reported techniques are not suitable for applications in food industries due to the utility of inorganic solvents and chemical compounds, in addition to they are expensive and complicated. For these reasons, alternative organic chemicals and solvents or green synthesized nanoparticles were developed to overcome the inactivation of free nisin by many food components through protecting nisin and releasing it in sustained manner [ 13 ]. For instance, acetic acid, a well-known biocompatible organic acid, has no adverse effects, no dietary restrictions and it is generally recognized as a safe food additive. This organic acid is commonly used, as a natural preservative, in the preservation of food especially in cheese and dairy products where it inhibit the development of bacteria, yeast and fungi [ 14 , 15 ]. Besides acetic acid, tween 80 has a great potential to stabilize nanoparticles dispersion through formation of a protective coat around the nanoparticles, so it was used in food without adverse health effect [ 16 , 17 ].
Application of nisin in dairy industry was reported in more than 55 countries due to its prominent antimicrobial, technological characteristics, safety, stability and flavorless. Commercially, nisin was used in several food matrices to ensure safety, extend shelf life, and to improve the microbial quality either through addition of nisin directly in its purified form or through its production in situ by live bacteria [ 18 , 19 , 20 ]. For instance, nisin was added as a bio-preserving ingredient in some kinds of cheese [ 21 , 22 , 23 ], skim milk and whole milk [ 24 , 25 , 26 , 27 ]. Nisin has a potent antibacterial effect against spore-forming bacteria that are the main spoilage concerns in the food industry [ 26 ]. However, several factors such as neutral pH [ 4 ], Fat% [ 25 ], protein% [ 28 ] as well as calcium and magnesium concentrations that can reduce the antimicrobial efficacy of nisin were reported when used directly in dairy foods [ 15 , 29 , 30 ]. Certain previously reported strategies, such as encapsulation and nano-encapsulation of nisin, were applied to increase the antimicrobial efficacy of nisin in dairy industry [ 31 , 32 ]. . Importantly, there is no available data about the use of nisin or nisin NPs as antimicrobial agents during yoghurt preparation.
Accordingly, the current study was designed to prepare nisin NPs by simple nanoprecipitation technique using natural, biocompatible and safe materials. Also the aims of this study were extended to investigate the antibacterial effect of obtained nanoparticles on MRSA and E.coli O157:H7 during manufacturing and storage of yoghurt. Additionally, the effect of the used nisin NPs on the organoleptic properties of yoghurt was addressed.
Materials and methods
Acetic acid (Merck Co., Germany), nisin (Sigma Aldrich from Lactococcus lactis , potency ≥ 900 IU/mg, purity ≥ 95%, CAS Number 1414-45-5), Brain Heart Infusion (BHI) (BBL 11,407, USA), phosphate buffer saline (PBS) (Oxoid, Basingstoke, UK) were purchased and used as received. Polyethylene glycol sorbitan monooleate (Tween 80) was purchased from Sigma Aldrich. Additionally, Mueller Hinton agar (M173) was purchased from HiMedia (Pvt., India), and LAB204 Neogen Company. While, 0.5 McFarland Standard (8.2 log 10 CFU/ml) (Cat. No. TM50) was purchased from Dalynn Biologicals Co. The deionized water was obtained from the Molecular Biology Unit, Assiut University, Egypt.
Preparation of nisin nanoparticles
Nisin (2 mg/mL) was completely dissolved in 100 mL of 0.1 M aqueous acetic acid solution with the aid of sonication using cold probe sonication (UP100H Hielscher Ultrasound). Then, 50 mL of deionized distilled water was gradually added to the nisin solution while maintaining the pH value within the range of 2.5 to 3. Further, 0.01% tween 80 was added as a stabilizer and the mixture was constantly stirred at 25 oC for 7 h to eliminate acetic acid as much as possible. Finally, the nanoparticles suspensions were then sonicated for 5 min before stored at refrigerator temperature for further use. The obtained nanoparticles were examined for size, shape, antibacterial activity and stability after six months.
Characterization of the prepared nisin NPs
Dynamic light scattering (dls).
The prepared nanoparticles was characterized by DLS at a fixed scattered angle of 90° using a Zetasizer, ZS 90 (3000 HS, Malvern Instruments, Malvern, UK) at the Nanotechnology Unit, Al-Azhar University at Assiut, Egypt. Measurements were taken at 25 °C and Zetasizer® software (version 7.03) was used to collect and analyze the data [ 33 ].
Fourier-transform infrared spectroscopy (FTIR)
FTIR was performed at the Chemistry Department at the Faculty of Science, Assiut University. This experiment was used to identify the functional groups and the fingerprint of the molecule. Samples were prepared by compressing potassium bromide with either free nisin or NNPs into small discs. The produced discs were then scanned using FTIR spectrometer (FTIR, NICOLET, iS10, Thermo Scientific) in the wave number ranged from of 4000 to 500 cm − 1 [ 34 ].
High resolution transmission electron microscopy (HRTEM)
The morphology of the prepared nisin NPs was determined using HRTEM (JEM2100, Jeol, Japan) at the Electronic Microscope Unit, National Research Center, Egypt. The sample was diluted with deionized water, and a small drop of nisin NPs was dropped onto 200-mesh copper coated grids at room temperature and negatively stained with uranyl acetate for 3 min. Excess liquid was removed using Whatman filter paper and samples were dried at room temperature [ 35 ].
Bacterial strains and inoculum preparation
The tested pathogens (MRSA and E. coli O157:H7) were previously isolated from dairy products (milk, cheese and yoghurt) samples by culture method and identified using conventional biochemical method and PCR at a certified food lab, Animal Health Research Institute (AHRI), Egypt [ 36 , 37 ]. These isolates were inoculated in trypticase soy broth (Himedia, India) and incubated at 37˚C for 24 h, then co-cultured on selective agars such as MRSA agar base (Acumedia, 7420, USA) and Sorbitol MaCconkey agar (Himedia, India) [ 38 , 39 ] for MRSA and E. coli O157:H7, respectively. The isolates were inoculated in BHI broth and incubated at 37 °C for 24 h until turbidity was comparable to a 0.5 McFarland turbidity standard. Before inoculating bacteria in milk, the inoculum was washed twice in PBS and then re-suspended in skim milk.
Determination of minimum inhibitory concentration (MIC) of free nisin and nisin nanoparticles against MRSA and E. Coli O157:H7
To determine the MIC of nisin NPs against MRSA and E.coli O157:H7, the agar well diffusion method was used according to Suresh et al. [ 40 ] with minor modifications. In brief, 0.1 mL of the previously prepared bacterial suspensions was spread on Mueller Hinton agar plates and left for 10 min to be absorbed. Then, 8 mm wells were punched into the agar plates for testing the antimicrobial activity of nanoparticles. One-hundred µl of different concentrations of free nisin and nisin NPs (from 0.0313 mg/mL to 2 mg/mL) were poured onto the wells. One well in each plate contained 100 µL of sterile deionized water was kept as a negative control. After overnight incubation at 35 ± 2 °C, the diameters of the inhibition zones were observed and measured in mm [ 41 ]. Each concentration was performed in triplicate.
Assessment of nisin nanoparticles cytotoxicity
The biocompatibility and the cytotoxicity of the nisin NPs were evaluated using a MTT assay against a Vero cell line after culture at 37 °C in a humidified incubator with 5% CO 2 in Dulbecco’s Modified Eagle’s Medium supplemented with 10% Fetal Bovine Serum. The cells were seeded into a 96-well plate at a density of 1 × 10 4 cells/well overnight before treatment. Different dilutions (0.5×MIC, MIC, 2×MIC, 4×MIC) of optimized nisin NPs were added to the seeded cells. Cells without nanoparticles served as control group. After 72 h, the consumed media was replaced with phosphate buffered saline, 10 µL from 12 mM MTT stock solution was added to each well and cells were incubated for 4 h at 37 °C. Next, 50 µL DMSO was added to dissolve formazan crystals and then the absorbance was measured at 570 nm using a BMG LABTECH®-FLUO star Omega microplate reader (Ortenberg, Germany). All experiments were performed in triplicate.
Antibacterial efficacy of the free nisin and nisin NPs against MRSA and E. Coli O157:H7 during manufacturing and storage of yoghurt
Fresh milk was heated at 85 °C for 5 min in water bath then suddenly cooled. The prepared inoculums were added to the warmed milk (41 ºC) in a count of 10 6 CFU/mL. The inoculated milk was divided into four parts for further use as following, part 1 is the positive control (contained MRSA or E. coli O157:H7 only, one jar each), part 2 (contained MRSA or E. coli O157:H7 with nisin NPs at MIC and 2×MIC, two jars each), part 3 (contained MRSA or E. coli O157:H7 with free nisin at MIC and 2×MIC, two jars each) and part 4 (negative control; free from pathogens and contained free nisin or nisin NPs only, one jar each). After inoculation of the different treatments, yoghurt was manufactured according to Sarkar [ 42 ] by adding 2% yoghurt starter culture ( Streptococcus thermophilus and Lactobacillus delbrueckii subsp. bulgaricus ) at 41 °C to milk. The prepared yoghurt was placed in a constant-temperature incubator at 40 °C until pH reached 4.6 to 4.5. Finally, the obtained products were stored at refrigeration temperature (4 ± 1 °C) for 5 days. Samples were collected just after manufacturing of yoghurt and every 2 days during storage, then tested for the count of MRSA using MRSA agar base media [ 43 ], and E. coli O157:H7 using Sorbitol MacConkey (SMAC) agar plates [ 44 ]. In addition, pH values were determined in the examined samples as previously described by Igbabul et al. [ 45 ]. In brief, 10 g o f yoghurt sample was dissolved in 100 mL of distilled water. The mixture was left to equilibrate at room temperature. Then, the pH of the samples was then measured by a pH meter (Microprocessor pH meter, pH 537, WTW, Germany).
Organoleptic assay of manufactured yogurt
Pathogen-free yoghurt jars (negative control) were prepared with two concentrations of either free nisin or nisin NPs (MIC and 2×MIC) as previously mentioned to be used for organoleptic evaluation. Thirty-five panelists were selected in teams of different ages, sex and education. The perception of consumers toward samples with two concentrations of nisin NPs was recorded. Consumers were asked to evaluate the color, flavor, mouth feel, appearance, and overall acceptability (OAA) of the prepared yoghurt samples containing nisin NPs [ 46 ]. The scale points were excellent (5); very good (4); good (3); acceptable (2); and poor (1).
Statistical analysis
One-way analysis of variance (ANOVA) was performed using the SPSS program (SPSS Inc., Chicago, IL, USA, 18) to determine the statistical significance of differences between groups. Results with P < 0.05 were considered statistically significant. The microbiological and cytotoxicity assay data were prepared using Excel software version 2017. While, the FTIR results were performed using Origin Lab 2021 for graphing and analysis. All experiments were carried out in triplicate.
Characterization of the prepared nanoparticles
The freshly prepared nisin NPs had 26.55 nm size and PDI 0.227 as determined by zetasizer. While, the diameter of the same after 6 months at refrigeration temperature was 86.50 nm with a PDI equal to 0.431 (Table 1 ). These results indicated that reasonable small-sized particles of nisin were obtained by precipitation technique using acetic acid. The small size of the prepared particles and the small PDI range (from 0.2 to 0.4) indicated a mono size dispersion and a good stability of the prepared nisin NPs.
The size and morphology of the freshly prepared nisin NPs and after 6 months of storage were measured by HRTEM are presented in Fig. 1 . Both freshly prepared and stored nisin NPs were approximately uniform in size with adequate distribution of particles. The shape of the particles was nearly spherical with slightly a bit of agglomeration just after 6 months of storage. The average size of freshly prepared nisin NPs was 7.35 nm while, after 6 months was 15.4 nm. The size of particles determined by TEM is usually smaller than the dynamic particles determined by zeta-sizer because TEM determine the actual particle diameter while zeta-sizer determine the particles diameter with adjacent moving layers of solvents.

The TEM images of freshly prepared nisin NPs (A) and after 6th months of storage (B)
Figure 2 showed the FTIR of pure and nisin NPs; both spectrum showed the characteristic peaks of nisin at 3425, 1599 and 1493 cm − 1 corresponded to O-H stretching of COOH, C = O stretching of amide I and N-H bending amide II. Bands 1530 cm − 1 in free nisin indicated the stretching of amid II and which, increased to 1549 cm − 1 in nisin NPs that indicated increase the H- bond in nano form than free one. The results of FTIR spectrum confirmed that the formation of nisin NPs did not result in any chemical changes or interaction of nisin with used the materials. These results also demonstrated the suitability of the applied method for the preparation of chemically stable and small-sized nisin NPs.
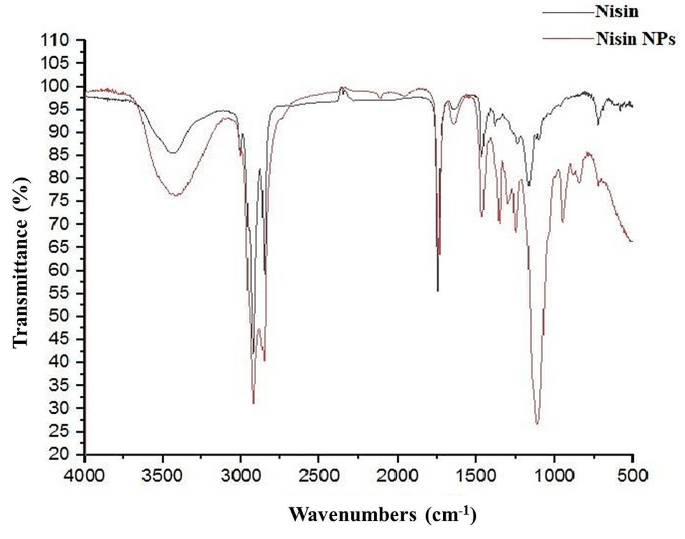
The FTIR of pure nisin and nisin NPs
Assessment of Nisin nanoparticles cytotoxicity
In the present study, Veros cells were exposed to nisin NPs for 48 and 72 h, and the cytotoxicity was measured by MTT assays. Results showed that the MIC did not exhibit an anti-proliferation effect (Fig. 3 ). Interestingly, even at very high concentrations (4xMIC), there were no cytotoxicity effect as the percentage of viable cells reach 92% and 89.98% after 48 and 72 h, respectively. The obtained findings confirmed the safety and good biocompatibility of the prepared nisin NPs at MIC level.
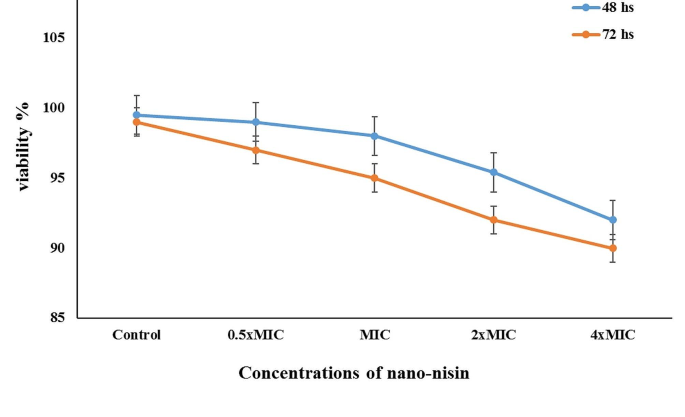
Cytotoxicity and cell viability of different concentrations nisin NPs using Vero cells after 48 and 72 h using MTT assay
MIC of free nisin and nisin NPs against MRSA and E. Coli O157:H7
The efficacy of the free nisin and prepared nisin NPs against MRSA and E. coli O157:H7 was investigated using agar well diffusion assay (Table 2 ). Nisin and its nanoparticles showed potent antibacterial effect against MRSA than E. coli O157:H7. The MICs of nisin and nisin NPs toward MRSA were 0.0625 and 0.0313 mg/mL, respectively. While, 0.125 mg/mL was the MIC of both nisin and nisin NPs against E. coli O157:H7. Of note, growth inhibition zone was not observed against MRSA at 0.0313 mg/mL of nisin, and toward E. coli O157:H7 at both 0.0625 and 0.0313 mg/mL nisin (Table 2 ). On the other hand, the prepared nisin NPs could produce inhibition zones against MRSA with a mean diameter ranged from 25.4 ± 2.1 mm to 7.1 ± 0.89 mm at concentrations of 2 to 0.0313 mg/mL, respectively. Also, the nisin NPs showed anti- E. coli O157:H7 activity at different concentrations of 2, 1, 0.5, 0.25 and 0.125 mg/mL with average size of 20.1, 15.4, 12.7, 9.5 and 7.2 mm of the inhibitory zones, respectively. There were no inhibition zones against E. coli O157:H7 at 0.0625 and 0.0313 mg/mL of nisin NPs. Overall, the obtained findings indicated that the most effective MICs of nisin and nisin NPs for both organisms were 0.125 mg/mL (Table 2 ).
Antibacterial effect of nisin and nisin NPs against MRSA and E. Coli O157:H7 during manufacturing and storage of yoghurt
Figure 4 presented the antibacterial activity of nisin against the examined foodborne pathogens (MRSA and E. coli O157:H7). Here, nisin at 0.125 and 0.25 mg/ml could induce antibacterial effect against MRSA (3.3 and 3 log 10 CFU/g, respectively) after 24 h of yoghurt storage. However the effect was not higher as in case of nisin NPs (2.3 and 1 log 10 CFU/g) at the same concentrations and time of storage. While, the inhibitory impact of the free nisin on E. coli O157:H7 was observed after 24 h (3.7 log 10 CFU/g) and 3 days (3.8 log 10 CFU/g) of storage at the concentrations of 0.25 and 0.125 mg/mL, respectively. The pathogens were still detected till the end of the experiment in nisin treated yoghurt (Fig. 4 ).
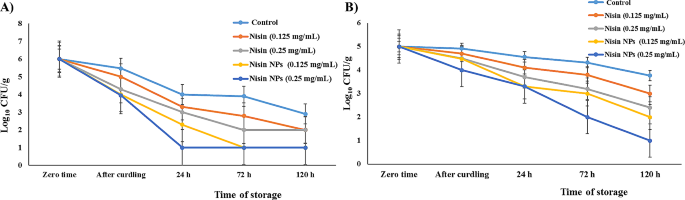
Antibacterial effect of free nisin (A) and nisin NPs (B) on MRSA and E.coli O157:H7 during manufacturing and storage of yoghurt
On the other hand, there was a clear reduction in mean count of MRSA and E.coli O157:H7 in the laboratory-manufactured yoghurt supplemented with different concentrations (0.125 and 0.25 mg/mL) of nisin NPs. A complete inhibition of MRSA was observed after 24 h and at the 3rd day of storage by 0.25 and 0.125 mg/mL of nisin NPs, respectively (Fig. 5 ). While, E. coli O157:H7 was undetectable at the 5th day of storage with 0.25 mg/mL nisin NPs, however it was still detected till the end of the experiment in either yoghurt inoculated with 0.125 mg/mL nisin NPs or in the positive control group (Fig. 4 ). Taken together, the antimicrobial count tests revealed that the free nisin is not effective as the nisin NPs at same time points during processing and storage of yoghurt.
During storage, the pH did not change significantly between different treatments. However, the negative control group showed little decrease in pH in comparison to other groups at the 3rd and 5th day of storage (3.5 and 3, respectively).
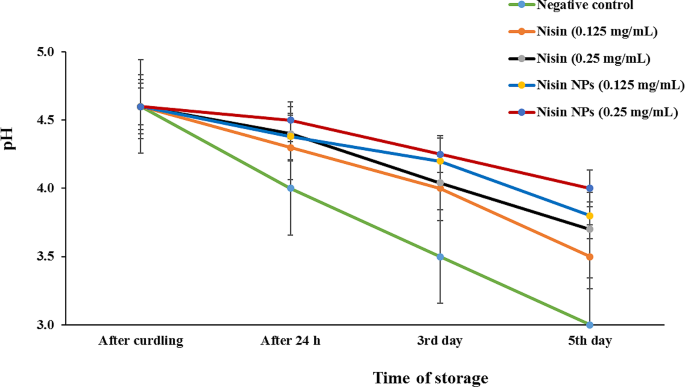
Evaluation of pH levels during processing and storage of yoghurt inoculated with different concentrations of free nisin or nisin NPs
Organoleptic evaluation of the laboratory-manufactured yoghurt
Figure 6 clarified that there was no difference in the sensory properties between the different groups (contained 0.125 or 0.25 mg/mL nisin (Fig. 6A) or nisin NPs (Fig. 6B)) in comparison to the control group. The OAA of yoghurt inoculated with 0.125 mg/mL and 0.25 mg/mL of free nisin was 3 and 2.5, respectively (Fig. 6A). While, the control samples had the highest score in mouth feel (4.5), followed in order with yoghurt loaded with 0.125 mg/mL and 0.25 mg/mL nisin NPs (3.8 and 2.7, respectively). Additionally, the overall acceptability (OOA) of control, 0.125 mg/mL and 0.25 mg/mL nisin NPs groups was 4, 3.7 and 3, respectively (Fig. 6B). Such findings indicated the high acceptability of yoghurt containing different concentrations of nisin NPs than those inoculated with free nisin.
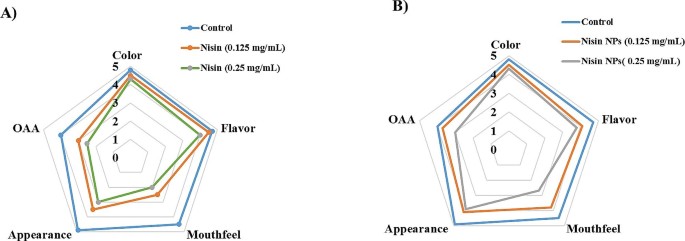
Organoleptic properties of yoghurt inoculated with different concentrations of free nisin and nisin NPs
The current study elucidated for the first time the inhibitory effect of free nisin and nisin NPs on two of the most common foodborne pathogens (MRSA and E. coli O157:H7) during processing and storage of laboratory manufactured yoghurt. Strikingly, adding of nisin NPs to yoghurt could induce much higher antibacterial effect on MRSA and E. coli O157:H7 with high consumer acceptability than free nisin. Accordingly, nisin NPs could be a useful and effective bio-preservative candidate against MRSA and E. coli O157:H7 in dairy industry.
The present study revealed that nisin NPs was prepared by a novel and safe method using natural material such as acetic acid which is commonly applied in food products. Chang et al. [ 47 ]. prepared ultra-small sizes of nisin NPs by nanoprecipitation method using HCL while we obtained much smaller particle size of NNPs using acetic acid which is more safer, less toxic and accepted by consumers. The particle size determined by TEM is smaller than the size measured by DLS this difference could be attributed to the removal of solvent and shrinking of nanoparticles during the drying of nisin NPs samples for TEM investigations. In addition, DLS measures the hydrodynamic diameter of the dispersed moving particles with the surrounding moving layers of solvents [ 48 , 49 ].
The result of FTIR was in consistent with that of Flynn et al. [ 50 ]. Herein, we found that the -OH stretching peak of nisin NPs displayed a greater intensity than that of free nisin, which indicated a stronger hydrogen bonding formation within nisin NPs. In case of free nisin, the peak at 1620 cm − 1 corresponding to COO − was shifted to 1610 cm − 1 in nisin NPs indicating that the hydrogen bonding was increased within nisin NPs. In contrast, the amid II band in free nisin appeared at 1530 cm − 1 became more obvious at 1549 cm − 1 in nisin NPs which was in agreement with Webber et al. [ 51 ]. . Band of amide I at wave number of 1632 cm − 1 could be due to the change in the structure of free nisin when converted into nisin NPs by using natural acetic acid.
In food chain, nisin has been approved for use in over 50 countries due to its safety and its potent antimicrobial activity without inducing microbial resistance [ 52 ]. Of particular note, the FAO/WHO Codex Committee and US FDA allow using nisin as a food additive in dairy products at a concentration up to 250 mg/kg [ 1 , 53 ]. Moreover, European Food Safety Authority [ 54 ] reported that nisin has been shown to be non-toxic to humans and it is safe as a food preservative for dairy and meat products. In the current study, the examined organisms (MRSA and E. coli O157:H7) have been involved in many food outbreaks worldwide as well as their resistance to many antibiotics, considered a challenge to be controlled [ 55 , 56 , 57 ]. Therefore, the present study could be a useful alternative strategy to avoid the possible health hazards of these organisms after consumption of yoghurt using either nisin or nisin NPs as natural food preservatives.
The obtained results revealed that the MICs of nisin and nisin NPs against MRSA were lower than that of E. coli O157:H7. This could be due to the ability of nisin to penetrate the cell wall of Gram-positive bacteria, however, it is difficult for nisin to penetrate the outer membrane barrier of Gram-negative bacteria [ 58 ]. Nisin could destroy bacteria through two mechanisms, either by making pores in the plasma membrane or by inhibiting the cell wall biosynthesis through binding to lipid II [ 59 , 60 , 61 ]. Importantly, the obtained results in the current study showed that that MIC of nisin NPs against MRSA was lower than that of pure nisin. Similarly, Zohri et al. [ 62 ] reported that the MICs of nisin and Nisin-Loaded nanoparticles was 2 and 0.5 mg/mL after 72 h of incubation period with the S. aureus samples, respectively. In addition, Moshtaghi et al. [ 63 ] examined the antibacterial effect of nisin on S. aureus and E. coli at different pH values and they found that the MICs against S. aureus were ranged from 19 to 312 µg/mL of nisin at pH levels from 8 to 5.5, respectively. While for E. coli , the MICs were from 78 to 1250 µg/mL at the same range of pH, respectively [ 63 ].
Interestingly, nisin inhibited the pathogenic foodborne bacteria and many other Gram-positive food spoilage microorganisms [ 13 ]. In the present study, evaluation of the kinetic growth of MRSA and E. coli O157:H7 based on the total counts in the laboratory manufactured yoghurt revealed that nisin NPs was able to inhibit more effectively the growth of such foodborne pathogens than free nisin during manufacturing and storage of yoghurt. These findings were in concurrent with those obtained by Zohri et al. [ 62 ] who demonstrated that nisin-loaded chitosan/alginate nanoparticles showed more antibacterial effect than free nisin on the growth of S. aureus in raw and pasteurized milk samples. Additionally, nisin Z in liposomes can provide a powerful tool to improve nisin stability and inhibitory action against Listeria innocua in the cheddar cheese [ 64 ]. In our study, nisin NPs showed a complete inhibition of MRSA after curdling of yoghurt and reduced the survivability of E. coli O157:H7 when applied at two different concentrations during storage of such product. Nisin NPs with high specific surface area could be easily attached to the target cell surface leading to increased permeability of the cell membrane, and finally cause bacterial cell death. Furthermore, nisin NPs were thermo-tolerant because of the internal non-covalent interactions in the nanoparticles [ 4 , 65 ]. Additionally, the decline in the mean count of the examined pathogens (MRSA and E.coli O157: H7) in the current study may be due to the effect of low pH (high acidity) of yoghurt that leads to shrinkage and death of the bacterial cells [ 66 ]. Similarly, Al-Nabulsi et al. [ 67 ] reported that the combination of a starter culture, low temperature, and pH ( ∼ 5.2) had inhibitory effects on the growth of S. aureus .
The effect of adding different levels of nisin and nisin NPs on OAA scores of yoghurt was recorded and the obtained results were in agreement with Hussain et al. [ 68 ], Radha [ 3 ], and Gharsallaoui et al. [ 4 ] who reported that a Nigerian fermented milk product had acceptable sensory scores till 25th day of storage when loaded with nisin at 400 IU/mL. Additionally, Chang et al. [ 47 ] said that the thermal treatments are known to cause undesirable changes in the sensory, nutritional and/or technological properties of milk. Taking advantage of the antimicrobial action of nisin NPs against several spoilage and pathogenic microorganisms, this innovative non-thermal food preservative offers the inactivation of microorganisms with minimal impact on the quality, safety, nutritional values and acceptability of dairy products.
Overall, as the demand for preservative-free food products increased, natural antimicrobials have gained more and more attention because of their effectiveness and safety. Consequently, the current study investigated that the addition of nisin NPs to milk for manufacturing of yoghurt can be used as an innovative preventive measure to inhibit the contamination with foodborne pathogens. However, further researches are required to determine the effective and safe dose of nisin NPs for application in other dairy products.
The present study prepared nisin NPs using acetic acid by precipitation method and the obtained particles were small in size with good stability and consumer acceptability. The antibacterial effect of nisin and nisin NPs against MRSA and E. coli O157:H7 in yoghurt was impressive. Additionally, the studied nanoparticles did not affect the sensory and textural characteristics of the finished product. Hence, this study could be useful for yoghurt makers and dairy products factories through using this novel preservation technology to inhibit the growth of MRSA and E. coli O157:H7, in yoghurt and dairy products, and subsequently avoid food spoilage and foodborne diseases.
Data availability
All data and materials are available here in the current study.
Ibarra-Sánchez LA, El-Haddad N, Mahmoud D, Miller MJ, Karam L. Invited review: advances in nisin use for preservation of dairy products. J Dairy Sci. 2020;103(3):2041–52.
Article PubMed Google Scholar
Batiha G, Hussein DE, Algammal A, George T, Jeandet P, Al-Snafi A, Tiwari A, Pagnossa J, Gonçalves Lima CM, Thorat N et al. Application of Natural antimicrobials in Food Preservation: recent views. Food Control 2021, 126.
Radha K. Nisin as a biopreservative for pasteurized milk. Indian J Veterinary Anim Sci Res. 2014;10(6):436–44.
Google Scholar
Gharsallaoui A, Oulahal N, Joly C, Degraeve P. Nisin as a Food Preservative: part 1: Physicochemical Properties, Antimicrobial Activity, and Main uses. Crit Rev Food Sci Nutr. 2016;56(8):1262–74.
Article CAS PubMed Google Scholar
Gao S, Zhai X, Cheng Y, Zhang R, Wang W, Hou H. Starch/PBAT blown antimicrobial films based on the synergistic effects of two commercial antimicrobial peptides. Int J Biol Macromol. 2022;204:457–65.
FDA/HHS. Direct food substances affirmed as generally recognized as safe: nisin preparation. Fed Regulations. 1988;53:11247–51.
Thomas LV, Clarkson MR, Delves-Broughton J. In A. S. Naidu, editor, Nisin: Natural food antimicrobial systems (Florida, Boca Raton: CRC) 2000:Press, 463–524.
Pimentel-Filho Nde J, Martins MC, Nogueira GB, Mantovani HC, Vanetti MC. Bovicin HC5 and Nisin reduce Staphylococcus aureus adhesion to polystyrene and change the hydrophobicity profile and Gibbs free energy of adhesion. Int J Food Microbiol. 2014;190:1–8.
Thébault P, Ammoun M, Boudjemaa R, Ouvrard A, Steenkeste K, Bourguignon B, Fontaine-Aupart M-P. Surface functionalization strategy to enhance the antibacterial effect of nisin Z peptide. Surf Interfaces. 2022;30:101822.
Article Google Scholar
Liu G, Nie R, Liu Y, Mehmood A. Combined antimicrobial effect of bacteriocins with other hurdles of physicochemic and microbiome to prolong shelf life of food: a review. Sci Total Environ. 2022;825:154058.
Brum LFW, Dos Santos C, Zimnoch Santos JH, Brandelli A. Structured silica materials as innovative delivery systems for the bacteriocin nisin. Food Chem. 2022;366:130599.
Kazemzadeh S, Abed-Elmdoust A, Mirvaghefi A, Hosseni Seyed V, Abdollahikhameneh H. Physicochemical evaluations of chitosan/nisin nanocapsulation and its synergistic effects in quality preservation in tilapia fish sausage. J Food Process Preserv. 2022;46(3):e16355.
Article CAS Google Scholar
Elsherif W, Zeinab A-E. Effect of nisin as a biopreservative on shelf life of pasteurized milk. Assiut Veterinary Med J. 2019;65:1–24.
Hu Y, Wu T, Wu C, Fu S, Yuan C, Chen S. Formation and optimization of chitosan-nisin microcapsules and its characterization for antibacterial activity. Food Control. 2017;72:43–52.
Khan I, Oh D-H. Integration of nisin into nanoparticles for application in foods. Innovative Food Sci Emerg Technol. 2016;34:376–84.
Zhao Y, Wang Z, Zhang W, Jiang X. Adsorbed Tween 80 is unique in its ability to improve the stability of gold nanoparticles in solutions of biomolecules. Nanoscale. 2010;2(10):2114–9.
Bekhit M, Abu el-naga MN, Sokary R, Fahim RA, El-Sawy NM. Radiation-induced synthesis of tween 80 stabilized silver nanoparticles for antibacterial applications. J Environ Sci Health Part A. 2020;55(10):1210–7.
Cui HY, Wu J, Li CZ, Lin L. Anti-listeria effects of chitosan-coated nisin-silica liposome on Cheddar cheese. J Dairy Sci. 2016;99(11):8598–606.
Kondrotiene K, Kasnauskyte N, Serniene L, Gölz G, Alter T, Kaskoniene V, Maruska AS, Malakauskas M. Characterization and application of newly isolated nisin producing Lactococcus lactis strains for control of Listeria monocytogenes growth in fresh cheese. LWT. 2018;87:507–14.
Santos JCP, Sousa RCS, Otoni CG, Moraes ARF, Souza VGL, Medeiros EAA, Espitia PJP, Pires ACS, Coimbra JSR, Soares NFF. Nisin and other antimicrobial peptides: production, mechanisms of action, and application in active food packaging. Innovative Food Sci Emerg Technol. 2018;48:179–94.
Van Tassell ML, Ibarra-Sánchez LA, Takhar SR, Amaya-Llano SL, Miller MJ. Use of a miniature laboratory fresh cheese model for investigating antimicrobial activities. J Dairy Sci. 2015;98(12):8515–24.
Ibarra-Sánchez LA, Van Tassell ML, Miller MJ. Antimicrobial behavior of phage endolysin PlyP100 and its synergy with nisin to control Listeria monocytogenes in Queso Fresco. Food Microbiol. 2018;72:128–34.
Feng Y, Ibarra-Sánchez LA, Luu L, Miller MJ, Lee Y. Co-assembly of nisin and zein in microfluidics for enhanced antilisterial activity in Queso Fresco. LWT. 2019;111:355–62.
Jung D-S, Bodyfelt FW, Daeschel MA. Influence of Fat and emulsifiers on the efficacy of Nisin in inhibiting Listeria monocytogenes in Fluid Milk1. J Dairy Sci. 1992;75(2):387–93.
Bhatti M, Veeramachaneni A, Shelef LA. Factors affecting the antilisterial effects of nisin in milk. Int J Food Microbiol. 2004;97(2):215–9.
Saad MA, Ombarak RA, Abd Rabou HS. Effect of nisin and lysozyme on bacteriological and sensorial quality of pasteurized milk. J Adv Veterinary Anim Res. 2019;6(3):403–8.
Chen H, Zhong Q. Lactobionic acid enhances the synergistic effect of nisin and thymol against Listeria monocytogenes Scott A in tryptic soy broth and milk. Int J Food Microbiol. 2017;260:36–41.
Wirjantoro TI, Lewis MJ, Grandison AS, Williams GC, Delves-Broughton J. The effect of nisin on the keeping quality of reduced heat-treated milks. J Food Prot. 2001;64(2):213–9.
Silva CCG, Silva SPM, Ribeiro SC. Application of Bacteriocins and protective cultures in dairy food preservation. Front Microbiol. 2018;9:594.
Article PubMed PubMed Central Google Scholar
Houlihan AJ, Russell JB. The effect of calcium and magnesium on the activity of bovicin HC5 and nisin. Curr Microbiol. 2006;53(5):365–9.
da Silva Malheiros P, Daroit DJ, da Silveira NP, Brandelli A. Effect of nanovesicle-encapsulated nisin on growth of Listeria monocytogenes in milk. Food Microbiol. 2010;27(1):175–8.
Martinez RCR, Alvarenga VO, Thomazini M, Fávaro-Trindade CS, Sant’Ana AS. Assessment of the inhibitory effect of free and encapsulated commercial nisin (Nisaplin®), tested alone and in combination, on Listeria monocytogenes and Bacillus cereus in refrigerated milk. LWT - Food Sci Technol. 2016;68:67–75.
Lu P-J, Fu W-E, Huang S-C, Lin C-Y, Ho M-L, Chen Y-P, Cheng H-F. Methodology for sample preparation and size measurement of commercial ZnO nanoparticles. J Food Drug Anal. 2018;26(2):628–36.
Bi S, Ahmad N. Green synthesis of palladium nanoparticles and their biomedical applications. Materials Today: Proceedings 2022, 62:3172–3177.
Gruskiene R, Krivorotova T, Staneviciene R, Ratautas D, Serviene E, Sereikaite J. Preparation and characterization of iron oxide magnetic nanoparticles functionalized by nisin. Colloids Surf B. 2018;169:126–34.
Zakaria IM, Elsherif WM. Bactericidal effect of silver nanoparticles on methicillin resistant Staphylococcus aureus (MRSA) isolated from bulk milk tanks. Anim Health Res J. 2018;6(3):42–51.
Elsherif W, Ali DN. Antibacterial effect of silver nanoparticles on antibiotic resistant E. Coli O157:H7 isolated from some dairy products. Bulgarian J Veterinary Med 2020:442.
Bennett RW, Lancette GA. Detection of Staphylococcus aureus in food samples. Bacteriological Analytical Manual (BAM), Ch. 12./ FoodScience Research /Laboratory Methods/ucm071429htm 2016.
Sancak YC, Sancak H, Isleyici O. Presence of Escherichia coli O157 and O157:H7 in raw milk and Van Herby cheese. Bull Veterinary Inst Pulawy 2015, 59.
Suresh S, Karthikeyan S, Saravanan P, Jayamoorthy K. Comparison of antibacterial and antifungal activities of 5-amino-2-mercaptobenzimidazole and functionalized NiO nanoparticles. Karbala Int J Mod Sci. 2016;2(3):188–95.
Hassanien AA, Shaker EM. Investigation of the effect of chitosan and silver nanoparticles on the antibiotic resistance of Escherichia coliO157:H7 isolated from some milk products and diarrheal patients in Sohag City, Egypt. Veterinary World. 2020;13(8):1647–53.
Article CAS PubMed PubMed Central Google Scholar
Sarkar S. Effect of Nisin on Techno- logical and microbiological characteristics of stirred Yoghurt. J Microbiol Microb Technol. 2016;1(1):6.
Sivaraman GK, Gupta S, Sivam V, Muthulakshmi T, Elangovan R, Perumal V, Balasubramanium G, Lodha T, Yadav A. Prevalence of S. Aureus and/or MRSA from seafood products from Indian seafood products. BMC Microbiol 2022, 22.
Anyanwu M, Cugwu I, Okorie-Kanu O, Ngwu M, Kwabugge Y, Chioma A, Chah K. Sorbitol non-fermenting Escherichia coli and E. Coli O157: prevalence and antimicrobial resistance profile of strains in slaughtered food animals in Southeast Nigeria. Access Microbiol 2022, 4.
Igbabul B, Hiikyaa O, Amove J. Effect of fermentation on the Proximate Composition and Functional Properties of Mahogany Bean (Afzelia africana) Flour. Curr Res Nutr Food Sci J. 2014;2:01–7.
Lawless H, Heymann H. Sensory Evaluation of Food Science Principles and Practices. Chapter 1, 2nd Edition, Ithaca, New York 2010: https://doi.org/10.1007/1978-1001-4419-6488-1005 .
Chang R, Lu H, Li M, Zhang S, Xiong L, Sun Q. Preparation of extra-small nisin nanoparticles for enhanced antibacterial activity after autoclave treatment. Food Chem. 2018;245:756–60.
Jahanshahi M, Babaei Z. Protein nanoparticle: a unique system as drug delivery vehicles. Afr J Biotechnol 2008, 7.
Krivorotova T, Cirkovas A, Maciulyte S, Staneviciene R, Budriene S, Serviene E, Sereikaite J. Nisin-loaded pectin nanoparticles for food preservation. Food Hydrocolloids. 2016;54:49–56.
Flynn J, Durack E, Collins MN, Hudson SP. Tuning the strength and swelling of an injectable polysaccharide hydrogel and the subsequent release of a broad spectrum bacteriocin, nisin A. J Mater Chem B. 2020;8(18):4029–38.
Webber JL, Namivandi-Zangeneh R, Drozdek S, Wilk KA, Boyer C, Wong EHH, Bradshaw-Hajek BH, Krasowska M, Beattie DA. Incorporation and antimicrobial activity of nisin Z within carrageenan/chitosan multilayers. Sci Rep. 2021;11(1):1690.
Shin JM, Gwak JW, Kamarajan P, Fenno JC, Rickard AH, Kapila YL. Biomedical applications of nisin. J Appl Microbiol. 2016;120(6):1449–65.
Sobrino-López A, Martín-Belloso O. Use of Nisin and other bacteriocins for preservation of dairy products. Int Dairy J. 2008;18(4):329–43.
European Food Safety Authority. Opinion of the scientific panel on food additives, flavourings, processing aids and materials in contact with food on a request from the commission related to the use of nisin (E 234) as a food additive. EFSA J. 2005;3146:1–16.
WHO. Monitoring of Antimicrobial Resistance. Report of an Intercountry Workshop. 2003 Oct 14–17; Tamil Nadu, India 2004.
Titouche Y, Akkou M, Houali K, Auvray F, Hennekinne JA. Role of milk and milk products in the spread of methicillin-resistant Staphylococcus aureus in the dairy production chain. J Food Sci. 2022;87(9):3699–723.
Eltokhy HE, Abdelsamei HM, El barbary H, Nassif, mZ. Prevalence of some pathogenic bacteria in dairy products. Benha Veterinary Med J. 2021;40(2):51–5.
Li Q, Montalban-Lopez M, Kuipers OP. Increasing the antimicrobial activity of Nisin-based lantibiotics against Gram-negative pathogens. Appl Environ Microbiol 2018, 84(12).
Hasper HE, Kramer NE, Smith JL, Hillman JD, Zachariah C, Kuipers OP, de Kruijff B, Breukink E. An alternative bactericidal mechanism of action for lantibiotic peptides that target lipid II. Sci (New York NY). 2006;313(5793):1636–7.
‘t Hart P, Oppedijk SF, Breukink E, Martin NI. New insights into Nisin’s antibacterial mechanism revealed by binding studies with synthetic lipid II analogues. Biochemistry. 2016;55(1):232–7.
Tol MB, Morales Angeles D, Scheffers DJ. In vivo cluster formation of nisin and lipid II is correlated with membrane depolarization. Antimicrob Agents Chemother. 2015;59(6):3683–6.
Zohri M, Alavidjeh MS, Haririan I, Ardestani MS, Ebrahimi SE, Sani HT, Sadjadi SK. A comparative study between the Antibacterial Effect of Nisin and Nisin-Loaded Chitosan/Alginate Nanoparticles on the growth of Staphylococcus aureus in Raw and pasteurized milk samples. Probiotics Antimicrob Proteins. 2010;2(4):258–66.
Moshtaghi H, Rashidimehr A, Shareghi B. Antimicrobial activity of Nisin and Lysozyme on Foodborne pathogens Listeria Monocytogenes, Staphylococcus Aureus, Salmonella Typhimurium, and Escherichia Coli at different pH. J Nutrtion Food Secur. 2018;3(4):193–201.
Benech RO, Kheadr EE, Laridi R, Lacroix C, Fliss I. Inhibition of Listeria innocua in cheddar cheese by addition of nisin Z in liposomes or by in situ production in mixed culture. Appl Environ Microbiol. 2002;68(8):3683–90.
Hegedüs I, Nagy E. Stabilization of activity of hemicellulase enzymes by covering with polyacrylamide layer. Chem Eng Process. 2015;95:143–50.
Normanno G, La Salandra G, Dambrosio A, Quaglia NC, Corrente M, Parisi A, Santagada G, Firinu A, Crisetti E, Celano GV. Occurrence, characterization and antimicrobial resistance of enterotoxigenic Staphylococcus aureus isolated from meat and dairy products. Int J Food Microbiol. 2007;115(3):290–6.
Al-Nabulsi AA, Osaili TM, AbuNaser RA, Olaimat AN, Ayyash M, Al-Holy MA, Kadora KM, Holley RA. Factors affecting the viability of Staphylococcus aureus and production of enterotoxin during processing and storage of white-brined cheese. J Dairy Sci. 2020;103(8):6869–81.
Hussain SA, Garg FC, Pal D. Effect of different preservative treatments on the shelf-life of sorghum malt based fermented milk beverage. J Food Sci Technol. 2014;51(8):1582–7.
Download references
Acknowledgements
The authors thank the nanotechnology research and synthesis unit at animal health research institute, Assiut, Egypt for their help in preparation of nanomaterials.
Not applicable.
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB).
Author information
Authors and affiliations.
Certified Food Lab, Nanotechnology Research and Synthesis Unit, Animal Health Research Institute (AHRI), Agriculture Research Center (ARC), Assiut,, Egypt
Walaa M. Elsherif
Faculty of Health Sciences Technology, New Assiut Technological University (NATU), Assiut, Egypt
Walaa M. Elsherif & Gamal M. Zayed
Department of Zoonoses, Faculty of Veterinary Medicine, Sohag University, Sohag, Egypt
Alshimaa A. Hassanien
Department of Pharmaceutics and Pharmaceutical Technology, Al-Azhar University, Assiut, Egypt
Gamal M. Zayed
Department of Food Hygiene, Safety and Technology, Faculty of Veterinary Medicine, Assiut University, Assiut, Egypt
Sahar M. Kamal
You can also search for this author in PubMed Google Scholar
Contributions
W.M.E., A.A.H., G.M.Z., and S.M.K. conceived and designed the experiment. W.M.E., A.A.H., G.M.Z., and S.M.K. collected the experimental data. W.M.E., A.A.H., and S.M.K. performed the microbiological analysis. A.A.H. and G.M.Z. performed the preparation and analysis of nanoparticles. W.M.E. and S.M.K. performed the statistical analysis. All authors interpreted the data. W.M.E. wrote the first draft of the manuscript. All authors reviewed the manuscript.
Corresponding author
Correspondence to Sahar M. Kamal .
Ethics declarations
Ethics approval and consent to participate, consent for publication, competing interests.
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Elsherif, W.M., Hassanien, A.A., Zayed, G.M. et al. Natural approach of using nisin and its nanoform as food bio-preservatives against methicillin resistant Staphylococcus aureus and E.coli O157:H7 in yoghurt. BMC Vet Res 20 , 192 (2024). https://doi.org/10.1186/s12917-024-03985-1
Download citation
Received : 12 October 2023
Accepted : 21 March 2024
Published : 11 May 2024
DOI : https://doi.org/10.1186/s12917-024-03985-1
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- E.coli O157:H7
- Nanoparticles
- Cytotoxicity
- Food preservative
BMC Veterinary Research
ISSN: 1746-6148
- General enquiries: [email protected]
Millennial vs. boomer budgets: How spending has changed for young adults in the last 30 years
- Business Insider looked at how adults between 25 and 34 spent their money in 1989 compared to 2022.
- The findings show us how prices and habits changed since boomers were young adults.
- Young adults today are spending less on alcohol and mortgage interest.

In 1989, you could see "Batman" and "When Harry Met Sally" in the movie theater. People wore brightly colored fashion and bought Nintendo's Game Boy consoles.
In 2022, many people were still working from home amid the pandemic's disruptions to the workplace. They were wearing a lot of athleisure, and perhaps venturing back to movie theaters — this time to see "The Batman."
In the intervening 33 years, how younger adults spend their money has changed dramatically. Business Insider analyzed spending data for adults aged 25 to 34 in 1989 — which covers part of the baby-boomer generation — and 2022 — which largely consists of millennials — on various kinds of food, housing, education, and more.
In 1989, people between 25 and 34 were spending more, when adjusted for inflation, on beef, alcohol, and homes they owned than this age group did in 2022.
Here's how expenditures looked between the two:
For this analysis, Business Insider compared average annual expenditures for households that were headed by 25- to 34-year-olds in 2022 to those in 1989. We used data from the Consumer Expenditure Surveys program published by the Bureau of Labor Statistics. BI calculated inflation-adjusted figures for 1989 using consumer price index data to put those costs into 2022 dollars.
We wanted to examine how spending for baby boomers when they were young adults compared to millennials who were around the same age in 2022.
The differences in average spending between young adults in 1989 and 2022 could be due to changes in prices or shifting habits.
Take a look at rented dwellings, for example. The consumer price index data for rent of primary residence suggests the increase between 1989 and 2022 can be largely explained by a rise in prices, but that data also implies that younger adults are more likely to rent an apartment rather than own a home.
Millennials and Gen Zers also have different habits and living situations than older generations. For example, millennials are finding it hard to become homeowners in the US and Gallup survey results show that adults under 35 who drink alcohol are consuming fewer drinks on average than those under 35 years ago.
Taken together, the data offers a window into how young adults' budgets have changed over the past three decades, either due to rising costs for things like healthcare, seafood, fresh fruits, housing, and used vehicles, or because of changing habits and lifestyles. Below is a closer look at what's going on.
Millennials are spending a lot more on healthcare and rented housing
Health-insurance spending stands out between the average adult aged 25 to 34 in 1989 compared to 2022. After adjusting for inflation, the average person in that age group spent $755 in 1989. In 2022, it was over 200% higher.
A BLS report from November 2023 by Grace Hill looked at the effects of the pandemic on healthcare spending overall and broken down by age groups and other groupings.
Related stories
"The only age groups to increase overall healthcare spending in 2020 were the 25–34- and 45–54-years age groups," the report stated. "These age groups had the largest increases in health insurance expenditures: the largest component in healthcare spending."
Additionally, younger adults were spending more on rent and related expenses in 2022 than younger adults were in 1989. Based on average data, this group was spending about 60% more on apartments and other rented housing.
Millennials are spending less on used vehicles and mortgage interest
In 2022, the average young adult spent more on gas and motor oil than this group in 1989. However, they weren't spending as much on used cars and trucks.
Data not adjusted for inflation shows that used car and truck expenditures increased more than the CPI for used cars and trucks between 1989 and 2022.
A December BLS report about consumer expenditures said households in general, not just among younger adults, were spending more in 2022 on rent and related expenses and owned homes than in 2021.
"High home prices, high mortgage lending rates, and particularly high rental rates for apartments placed upward pressure on spending over the year," the report said. "Mortgage interest and principal payments are essential expenditures for owned dwellings, and a rapidly changing mortgage environment sent an exogenous shock through the market."
The report added that the high average mortgage rate in 2022 led to "consumers on the margin out of owned dwellings and into the rental market."
Though BLS doesn't directly track price changes for owned housing, it estimates them with a measure of owners' equivalent rent of residences, which is up over 160% between 1989 and 2022. Meanwhile, younger adults' spending for owned dwellings was up over 120% before adjusting 1989 expenditures for inflation.
Younger adults in 2022 spent more money on fresh fruits, vegetables, and seafood
In 1989, people between 25 and 34 spent less on fresh fruits and vegetables — including processed vegetables — than those in this age range decades later. The average person in this cohort spent 71% more on fresh fruits in 2022 than their counterparts in 1989. Plus, they spent 22% more on fish and seafood in 2022 and 4% more on poultry.
While not the exact years we looked at for our analysis, a 2016 report from the Pew Research Center shed light on how eating habits changed between 1970 and 2014; there were notable increases in chicken and cheese consumption over that time.
We can also look at consumer price index data to see how inflation impacted food spending. Before adjusting 1989 data for inflation, younger adults in 2022 spent 304% more on fresh fruits than younger adults in 1989. Over that period, prices for fresh fruits, based on the CPI, were up by nearly 170%, meaning that while part of the change in spending between the two years can be explained by price increases, younger adults were also eating a lot more fresh fruit in 2022 than in 1989.
In 2022, younger adults spent less on alcohol, beef, and dairy products
Average annual spending data shows that the average younger adult in 2022 spent almost 40% less on beef than the average younger adult in 1989. They also spent about 55% less on fresh milk and cream. The 2016 Pew Research Center report also found that people were eating a lot less beef in 2014 than in 1970. The same was true for drinking milk.
Based on our analysis, the average adult between 25 and 34 spent more on nonalcoholic beverages and less on alcoholic beverages in 2022 than the average young adult in 1989. A Gallup post shows alcohol drinkers who were between 18 and 34 in 2021 to 2023, which would also include Gen Z , had an average of 3.6 alcoholic drinks in the past seven days. Between 2001 and 2003, the average consumption was 5.2 drinks among drinkers aged 18 to 34.
Our analysis found that younger adults in 2022 weren't spending as much on cereals and cereal products — which included "ready-to-eat and cooked cereals, pasta, flour, prepared flour mixes, and other cereal products such as cornmeal, corn starch, and rice" — as younger adults were in 1989. Based on reporting from multiple outlets, cereal has fallen in popularity while breakfast sandwiches , bars, and other items that are easy to eat on the go are now popular.
Watch: Millions of homes could flood the US housing market thanks to boomers
- Main content
share this!
May 11, 2024
This article has been reviewed according to Science X's editorial process and policies . Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
Research explores ways to mitigate the environmental toxicity of ubiquitous silver nanoparticles
by Oregon State University
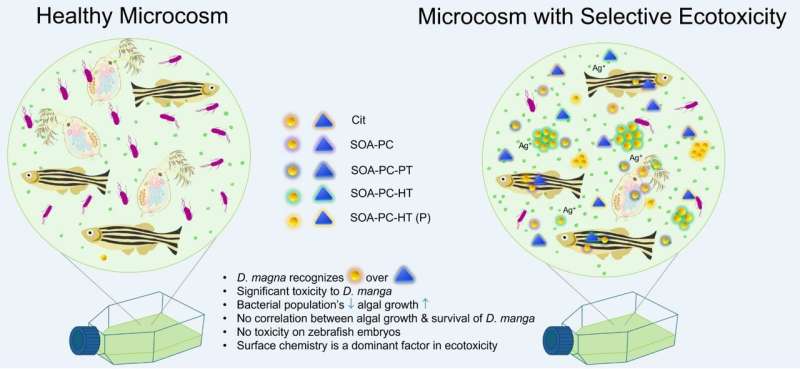
Silver has long been used to thwart the spread of illness and in recent years silver nanoparticles have been incorporated into products ranging from sanitizers, odor-resistant clothes and washing machines to makeup, food packaging and sports equipment.
Nanoparticles are tiny pieces of material ranging in size from one- to 100-billionths of a meter. In addition to their antimicrobial properties, silver nanoparticles are industrially important as catalysts and in electronics applications.
Despite their ubiquity, little is known about their environmental toxicity or how it might be mitigated.
Researchers at Oregon State University have taken a key step toward closing the knowledge gap with a study that indicates the particles' shape and surface chemistry play key roles in how they affect aquatic ecosystems.
The findings, published in Nanomaterials , are important because they suggest silver nanoparticles can be produced in formats that preserve their beneficial properties while limiting environmentally negative ones.
Scientists led by Marilyn Rampersad Mackiewicz and Stacey L. Harper assessed how spherical and triangular-shaped silver nanoparticles with five different surface chemistries affected their uptake and toxicity in a laboratory microcosm of bacteria, algae, Daphnia and embryonic zebrafish.
Daphnia are tiny crustaceans, and zebrafish are a small freshwater species that go from a cell to a swimming fish in about five days.
Zebrafish are particularly useful for studying the development and genetics of vertebrates, including the effects of environmental contaminants and pharmaceuticals on early embryonic development . They share a remarkable similarity to humans at the molecular, genetic and cellular levels; embryonic zebrafish are of special interest because in addition to developing quickly, they are transparent and can be easily maintained in small amounts of water.
The authors note that hundreds of tons of silver nanoparticles are produced every year for commercial uses, meaning it's inevitable some will end up in aquatic environments.
"Silver nanoparticles are not regulated by the Food and Drug Administration and not much is known about their toxicity except for the free silver ions that can result from surface oxidation of the nanoparticles," said Mackiewicz, assistant professor of chemistry. "Free silver ions are known to be toxic and in this paper we found a way to study the toxicity of silver nanoparticles and how they impact the environment irrespective of poisonous silver ions."
Mackiewicz, Harper and collaborators in the OSU colleges of Science, Engineering and Agricultural Sciences found silver nanoparticles negatively affect some species but not others.
"For example, there is a decrease in bacterial and Daphnia growth, and the size and shape of the particles can contribute to that, but the nanoparticles didn't affect zebrafish," she said. "And nanoparticles coated in lipids, organic compounds found in many natural oils and waxes, did not release significant amounts of silver ions—but they exhibited the greatest toxicity to Daphnia magna, the most sensitive species in the microcosm."
Overall, Mackiewicz said, the study showed that silver nanoparticles' shape and surface chemistry can be manipulated to achieve specific objectives necessary for better understanding and mitigating the risks associated with silver nanoparticles. A related study awaiting publication, she added, shows that small, spherical nanoparticles are more toxic than triangles or cubes.
Nanoparticles are the latest format, Mackiewicz notes, for an element that throughout history has been used to restrict the spread of human disease via incorporation into items used in everyday life. Its earliest recorded use for therapeutic purposes dates back 3,500 years.
During the Middle Ages, wealthy families used so many silver vessels, plates and other products that they developed bluish skin discolorations known as argyria, a condition believed to have led to the term "blue blood" as a description for members of the aristocracy.
Collaborating with Mackiewicz and Harper on the study were OSU researchers Bryan Harper and Arek Engstrom.
Provided by Oregon State University
Explore further
Feedback to editors

Tiger beetles fight off bat attacks with ultrasonic mimicry
59 minutes ago

Machine learning model uncovers new drug design opportunities
4 hours ago

Astronomers find the biggest known batch of planet ingredients swirling around young star

How 'glowing' plants could help scientists predict flash drought
5 hours ago

New GPS-based method can measure daily ice loss in Greenland

New candidate genes for human male infertility found by analyzing gorillas' unusual reproductive system
6 hours ago

Study uncovers technologies that could unveil energy-efficient information processing and sophisticated data security
7 hours ago

Scientists develop an affordable sensor for lead contamination
Chemists succeed in synthesizing a molecule first predicted 20 years ago

New optical tweezers can trap large and irregularly shaped particles
Relevant physicsforums posts, is it usual for vaccine injection site to hurt again during infection.
May 13, 2024
A Brief Biography of Dr Virgina Apgar, creator of the baby APGAR test
May 12, 2024
Who chooses official designations for individual dolphins, such as FB15, F153, F286?
May 9, 2024
The Cass Report (UK)
May 1, 2024
Is 5 milliamps at 240 volts dangerous?
Apr 29, 2024
Major Evolution in Action
Apr 22, 2024
More from Biology and Medical
Related Stories
Self-embedding silver nanoparticles: Researchers find the 'silver lining' in cotton gin waste
Apr 10, 2024
Researchers develop first of its kind, simple test for identifying toxic silver ions
Jul 15, 2020

Video: How silver nanoparticles cut odors
Sep 20, 2018
Silver nanoparticles show promise in fighting antibiotic-resistant bacteria
Jan 31, 2023
Panning for silver in laundry wastewater
Dec 20, 2017
Improving safety assessment of nanoparticles
Jan 4, 2023
Recommended for you

Uneven strain distribution induces detwinning in penta-twinned nanoparticles
9 hours ago
New gel breaks down alcohol in the body

Electron vortices in graphene detected for the first time
Nanoparticle plant virus treatment shows promise in fighting metastatic cancers in mice
High-speed atomic force microscopy helps explain role played by certain biomolecules in DNA wrapping dynamics
May 10, 2024

Designer peptoids mimic nature's helices
Let us know if there is a problem with our content.
Use this form if you have come across a typo, inaccuracy or would like to send an edit request for the content on this page. For general inquiries, please use our contact form . For general feedback, use the public comments section below (please adhere to guidelines ).
Please select the most appropriate category to facilitate processing of your request
Thank you for taking time to provide your feedback to the editors.
Your feedback is important to us. However, we do not guarantee individual replies due to the high volume of messages.
E-mail the story
Your email address is used only to let the recipient know who sent the email. Neither your address nor the recipient's address will be used for any other purpose. The information you enter will appear in your e-mail message and is not retained by Phys.org in any form.
Newsletter sign up
Get weekly and/or daily updates delivered to your inbox. You can unsubscribe at any time and we'll never share your details to third parties.
More information Privacy policy
Donate and enjoy an ad-free experience
We keep our content available to everyone. Consider supporting Science X's mission by getting a premium account.
E-mail newsletter
Delivery Hero in $1.25 Billion Deal With Uber for Foodpanda Taiwan Sale, Investment

Foodpanda riders get ready for deliveries outside a restaurant, amid the coronavirus disease (COVID-19) outbreak in Kuala Lumpur, Malaysia July 8, 2020. REUTERS/ Lim Huey Teng/File Photo
(Reuters) -Uber announced on Tuesday a $1.25 billion deal to take over Delivery Hero's foodpanda business in Taiwan and buy new shares in the German firm in a move that would boost liquidity of the delivery specialist grappling with rising competition in Asia.
Asia has become Delivery Hero's biggest market after its $4 billion deal in South Korea in 2019 but the company has been trying to divest some of its assets in the region to improve profitability.
While food delivery services in Asia have largely rebounded from a slowdown following the pandemic boom, many firms are now grappling with thin margins as they spend heavily in offering discounts and promotions to retain consumers who have become wary of rising inflation and cost of living.
"We need to focus our resources on other parts of our global footprint, where we feel we can have the largest impact for customers, vendors and riders," Niklas Ostberg, CEO and co-founder of Delivery Hero, said in a joint statement.
Under the deal, Uber will take over the foodpanda business in Taiwan for $900 million in cash and purchase $300 million in newly issued shares of Delivery Hero at 33 euros each, a 30% premium to its closing share price on Monday.
The U.S. company expects the acquisition to contribute at least $150 million annually to the adjusted core profit of its delivery business within a year of the deal's closing, which is likely in the first half of 2025.
Online food delivery platforms represent a small fraction of Taiwan's competitive food delivery market but the foodpanda operations in the island were break-even in terms of adjusted core earnings in the last 12 months ended March 31, the companies said.
The business processed transactions worth 1.6 billion euros ($1.73 billion) during that period.
REGULATORY RISK
Delivery Hero had been also looking to sell its foodpanda business in selected Southeast Asian markets as part of its restructuring. It said in February that it had terminated talks for the potential sale of those operations.
"With a better balance sheet and partnership with Uber, Delivery Hero's competitive situation has materially improved with restored ability to undergo marketing initiatives if required," JPMorgan analysts said in a client note.
But the analysts warned that Delivery Hero and Uber's combined 90% market share in the Taiwanese food delivery business could spark "regulatory risk."
Singapore's competition watchdog said last month it had looked into the likelihood of a potential deal between Grab Holdings and Delivery Hero, raising worries about competition in the food delivery market. But it closed the case after the talks had collapsed.
Delivery Hero said last month it would still look at any potential deal.
Grab and foodpanda control about 91% of Singapore's $2.5 billion food delivery market, according to a report by research firm Momentum Works, with Grab alone having a 63% market share.
($1 = 0.9271 euros)
(Reporting by Chandni Shah and Zaheer Kachwala in Bengaluru; Writing by Miyoung Kim; Editing by Nivedita Bhattacharjee and Subhranshu Sahu)
Copyright 2024 Thomson Reuters .
Tags: United States , Taiwan , Europe , Germany
The Best Financial Tools for You
Credit Cards

Personal Loans

Comparative assessments and other editorial opinions are those of U.S. News and have not been previously reviewed, approved or endorsed by any other entities, such as banks, credit card issuers or travel companies. The content on this page is accurate as of the posting date; however, some of our partner offers may have expired.

Subscribe to our daily newsletter to get investing advice, rankings and stock market news.
See a newsletter example .
You May Also Like
7 best reit etfs to buy for 2024.
Glenn Fydenkevez May 14, 2024

Roundtable Q&A on the Inflation Dilemma
Rachel McVearry May 14, 2024

7 Best International Stock Funds to Buy
Tony Dong May 14, 2024

7 Top Financial Advisor Firms by AUM
Marc Guberti May 14, 2024

Brokerage Account vs. IRA: Which Wins?
Wayne Duggan May 14, 2024

5 Great Fixed-Income Funds to Buy Now
Tony Dong May 13, 2024

7 High-Return, Low-Risk Investments
Brian O'Connell May 13, 2024

Best Vanguard ETFs to Buy

7 Best Equal-Weight ETFs to Buy
Glenn Fydenkevez May 13, 2024

These 3 Fund Families Control the Market
Wayne Duggan May 13, 2024

4 Sustainable Aviation Fuel (SAF) Stocks
Matt Whittaker May 10, 2024

Biggest Tech Companies in the World
Wayne Duggan May 10, 2024

7 Best Car Stocks to Invest in Now
Jeff Reeves May 10, 2024

5 Best Mutual Funds to Buy
Coryanne Hicks May 10, 2024

Fidelity Mutual Funds to Buy and Hold
Tony Dong May 10, 2024

Should You Buy Solana? 3 Pros, 3 Cons
Wayne Duggan May 9, 2024

7 Best Marijuana ETFs
Matt Whittaker May 9, 2024

10 Best-Performing ETFs of 2024
Jeff Reeves May 9, 2024

5 Best Gold Stocks to Buy Now
Glenn Fydenkevez May 9, 2024

9 Best Cheap Stocks to Buy Under $5
Ian Bezek May 9, 2024

MINI REVIEW article
This article is part of the research topic.
Catalysis and Sensing for our Environment
Research progress in the detection of trace heavy metal ions in food samples Provisionally Accepted

- 1 Beijing University of Chemical Technology, China
The final, formatted version of the article will be published soon.
Food safety is the basis for ensuring human survival and development. The threat of heavy metal ions to food safety has become a social concern with the rapid growth of the economy and the accompanying environmental pollution. Some heavy metal ions are highly toxic even at trace levels and pose significant health risks to humans. Therefore, ultrasensitive detection of heavy metal ions in food samples is important. In this mini-review, recent advances in the analytical methods based on nanomaterials for detecting trace heavy metal ions in food samples are summarized in three categories: electrochemical, colorimetric, and fluorescent methods. We present the features and sensing mechanisms of these three methods, along with typical examples to illustrate their application in the detection of heavy metal ions in foods. This mini-review ends with a discussion of current challenges and future prospects of these approaches for sensing heavy metal ions. The review will help readers understand the principles of these methods, thereby promoting the development of new analytical methods for the detection of heavy metal ions in food samples.
Keywords: Heavy metal ions, detection, Food samples, nanomaterials, Sensors
Received: 26 Apr 2024; Accepted: 13 May 2024.
Copyright: © 2024 Si, Wu, Jin and Wang. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY) . The use, distribution or reproduction in other forums is permitted, provided the original author(s) or licensor are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
* Correspondence: Mx. Yulong Jin, Beijing University of Chemical Technology, Beijing, 100029, Beijing Municipality, China Prof. Zhuo Wang, Beijing University of Chemical Technology, Beijing, 100029, Beijing Municipality, China
People also looked at
We've detected unusual activity from your computer network
To continue, please click the box below to let us know you're not a robot.
Why did this happen?
Please make sure your browser supports JavaScript and cookies and that you are not blocking them from loading. For more information you can review our Terms of Service and Cookie Policy .
For inquiries related to this message please contact our support team and provide the reference ID below.

IMAGES
VIDEO
COMMENTS
The effects of certain foods or dietary patterns on glycaemia, immune activation, and the gut microbiome may play a role in the relationships between food and mood. More research is needed to understand the mechanisms that link food and mental wellbeing and determine how and when nutrition can be used to improve mental health. 3 fig 1 4.
The effects of certain foods or dietary patterns on glycaemia, immune activation, and the gut microbiome may play a role in the relationships between food and mood. More research is needed to understand the mechanisms that link food and mental wellbeing and determine how and when nutrition can be used to improve mental health.
Poor nutrition may be a causal factor in the experience of low mood, and improving diet may help to protect not only the physical health but also the mental health of the population, say Joseph Firth and colleagues ... say Joseph Firth and colleagues Food and mood: how do diet and nutrition affect mental wellbeing? BMJ. 2020 Jun 29:369: m2382 ...
A meta-analysis including studies from 10 countries, conducted by researchers at Linyi People's Hospital in Shandong, China, suggests that dietary patterns may contribute to depression ( Psychiatry Research, Vol. 253, 2017), for example. Dietary patterns are also related to hippocampal volume in older adults, according to a study led by Felice ...
In this review, we will discuss the extent of, and mechanisms for, diet's influence on mood and cognition during different stages of life, with a focus on microglial activation, glucocorticoids ...
The effects of certain foods or die-tary patterns on glycaemia, immune activation, and the gut microbiome may play a role in the relationships between food and mood. More research is needed to under-stand the mechanisms that link food and mental wellbeing and determine how and when nutrition can be used to improve mental health. experiences.
Supporting this perspective of "food as well-being", recent research suggests that "healthy" food choices, such as eating more fruits and vegetables, have not only physical but also mental ...
But over the years, a growing body of research has provided intriguing hints about the ways in which foods may affect our moods. A healthy diet promotes a healthy gut, which communicates with the ...
Purpose of Review The question whether food choice and eating behavior influence the mood or are influenced by the mood has been inquisitive to scientists and researchers. The purpose of this review is to support or refuse the argument that mood is affected by food or vice versa. Recent Findings The association between food and mood has been comprehensively elucidated in this review based on ...
Add some high-fibre fare, fermented food and fish a few times a week, and you could be eating your way to better mental health, too. Those are the recommendations from nutritional psychiatry research.
Studies showing the interrelationships between food, mood, and diseases. The corresponsive relationship between food choices and mood status. In bad mode, the desire to unhealthy foods increases ...
Introduction. There is more to food than just nutrition. Past research has found that food intake is associated with an individual's affective states (Arnow et al., 1995, Macht, 2008).Many people eat in order to distract themselves from, compensate for, or cope with negative affects such as stress, anxiety, frustration, fear, daily hassles, sadness, boredom, depression, and fatigue (Chua et al ...
One idea that is of great importance is how the food we eat can affect our mood. It is possible that the components in food, such as vitamins and minerals, can influence depression. It also explores how depression can influence our food choices [ 4 ]. Figure 1 highlights the connections between what we eat and our mental and physical health.
Background Emotional eating is defined as a nonpathological eating behavior, whereas binge-eating disorder (BED) is defined as a pathological eating behavior. While different, both share some striking similarities, such as deficits in emotion regulation and inhibition. Previous research has suggested the existence of an "eating continuum" that might reflect the increased severity of ...
Do plan meals and snacks ahead of time. Do keep track of your eating habits. Do limit night eating. Do drink plenty of water. Staying hydrated helps your body operate at its best. Do delay ...
Eating high levels of ultra-processed foods linked with higher risk of death, study finds 04:04. New research is adding to the evidence linking ultra-processed foods to health concerns. The study ...
Understanding the mechanisms involved in food breakdown in the human gastrointestinal (GI) tract is essential in food digestion research. Research to study food digestion in the human GI tract requires in vivo and in vitro approaches. In vivo methods involving human or animal subjects are often cost-prohibitive and raise ethical concerns. For these reasons, in vitro approaches are becoming ...
Every year, 1.3 billion tonnes of food is wasted globally, the equivalent of one-third of all food produced for human consumption. Busy lives and cooking habits lead to neglecting fresh produce until it spoils, adding to the problem. New research finds that keeping a 'food log' for 6 weeks can reduce the amount of waste by an average of 108g per week, an effect that can still be seen six ...
Background Natural antimicrobial agents such as nisin were used to control the growth of foodborne pathogens in dairy products. The current study aimed to examine the inhibitory effect of pure nisin and nisin nanoparticles (nisin NPs) against methicillin resistant Staphylococcus aureus (MRSA) and E.coli O157:H7 during the manufacturing and storage of yoghurt. Nisin NPs were prepared using new ...
In 1989, people between 25 and 34 spent less on fresh fruits and vegetables — including processed vegetables — than those in this age range decades later. The average person in this cohort ...
Research explores ways to mitigate the environmental toxicity of ubiquitous silver nanoparticles. by Oregon State University. Credit: Nanomaterials (2024). DOI: 10.3390/nano14080654. Silver has ...
Reuters. Foodpanda riders get ready for deliveries outside a restaurant, amid the coronavirus disease (COVID-19) outbreak in Kuala Lumpur, Malaysia July 8, 2020.
Food safety is the basis for ensuring human survival and development. The threat of heavy metal ions to food safety has become a social concern with the rapid growth of the economy and the accompanying environmental pollution. Some heavy metal ions are highly toxic even at trace levels and pose significant health risks to humans. Therefore, ultrasensitive detection of heavy metal ions in food ...
Mexico's central bank kept borrowing costs unchanged Thursday after inflation reaccelerated last month, taking the remote possibility of a second straight interest rate cut off the table.